 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
- Acne & Acne Scarring
- Rosacea
- Psoriasis (includes Excimer laser, Narrow band UVB phototherapy)
- Eczema (Atopic Dermatitis)
- Seborrheic Dermatitis
- Contact Dermatitis
- Hives (Urticaria)
- Vitiligo (includes Excimer laser, Narrow band UVB phototherapy)
Hair Loss (Alopecia)
- Pruritus (Chronic Itching)
- Autoimmune Skin Disorders
- Warts, Molluscum, Fungal
- Sarcoidosis (Skin Involvement)
- Hyperhidrosis (Excessive Sweating)
- Lichen planus
- Blistering Skin Disorders
- Bacterial Skin Infections
- Keloids (Overgrown scar)
- Paraneoplastic Dermatoses (a clue to an internal cancer)
- Skin Issues Related to STDs (STIs)
- Scabies
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Hair Loss (Alopecia)
Overview
Hair loss (alopecia) is common—and there are many different causes. Some types are temporary and reversible, while others require early treatment to prevent permanent loss. The most important first step is an accurate diagnosis.
We evaluate hair loss in a medical, step-by-step way so you understand:
Why it’s happening
Whether it can grow back
Which treatments are most likely to help
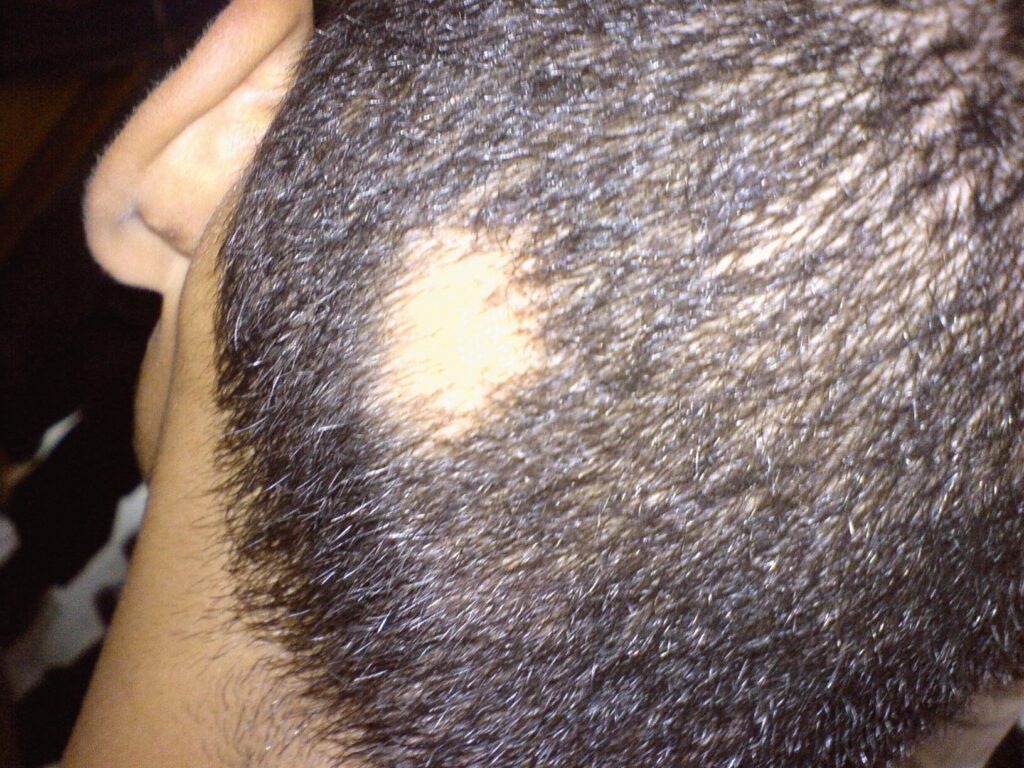
Common Types of Hair Loss We Diagnose
1) Pattern Hair Loss (Androgenetic Alopecia)
Gradual thinning over time
Often at the crown/part line in women or temples/crown in men
2) Telogen Effluvium (Shedding)
Increased shedding, often 2–3 months after a trigger such as illness, stress, surgery, childbirth, or medication changes
Usually temporary, but can last longer if triggers continue
3) Alopecia Areata
Sudden, patchy hair loss
Caused by an immune system attack on hair follicles
Can affect scalp, eyebrows, beard, or body hair
4) Scarring (Cicatricial) Alopecia
Inflammation damages hair follicles and can lead to permanent hair loss if not treated early
Often associated with burning, tenderness, scale, or “sore spots”
5) Traction Hair Loss
From tight hairstyles (braids, ponytails, extensions)
Often affects hairline/temples
Symptoms That Help Us Narrow the Cause
Tell us if you’ve noticed:
Sudden shedding vs gradual thinning
Itching, burning, pain, or scalp tenderness
Flaking, redness, bumps, or sores
Patchy loss vs diffuse thinning
Eyebrow/eyelash loss
Nail changes (sometimes linked with alopecia areata)
How We Evaluate Hair Loss
A typical evaluation may include:
Medical history (timing, triggers, medications, family history)
Scalp and hair exam (sometimes with dermoscopy/trichoscopy)
Hair pull test (gentle exam for shedding)
Lab work when appropriate (to check for common contributors like iron deficiency or thyroid issues)
Scalp biopsy (only when needed) to confirm diagnosis—especially if scarring alopecia is suspected
Treatment Options
Your plan depends on the diagnosis and your goals (regrowth, slowing loss, reducing shedding, scalp symptom relief).
1) For Pattern Hair Loss
Medical treatments to slow thinning and support growth
Long-term maintenance is often needed
2) For Telogen Effluvium
Identify and address the trigger
Support scalp health and hair cycling
Reassurance + follow-up (regrowth often takes time)
3) For Alopecia Areata
Anti-inflammatory/immune-modulating approaches, depending on severity and area affected
Treatment is often more effective when started early
4) For Scarring Alopecia
Goal is to stop inflammation and prevent further loss
Early diagnosis is crucial; regrowth may be limited where follicles are scarred
5) For Traction Hair Loss
Change hair practices (reduce tension)
Treat inflammation early to prevent permanent thinning
Pre-Op Instructions (Before Your Hair Loss Appointment)
(Not surgery—these are “before your visit” tips.)
1–2 weeks before your visit
Take photos of your hair/scalp in the same lighting (front, sides, crown, part line) to track change over time.
Write down:
When it started and whether it’s worsening
Any illness, stress, pregnancy, surgery, crash dieting, or new meds in the past 3–6 months
Family history of hair loss
Hair practices (tight styles, heat, extensions, chemical treatments)
48 hours before
If possible, avoid starting new hair supplements or treatments right before your visit (it helps us interpret what’s going on).
- If you use camouflage fibers or scalp concealer, try not to use them on the day of your exam.
Day of visit
Come with clean, dry hair if you can (minimal styling products helps us see the scalp clearly).
Bring:
A list of medications and supplements
Recent lab results (if you have them)
Your shampoos/serums (photos of labels are fine)
Post-Op Instructions (After Evaluation or Treatment)
After starting a hair loss treatment plan
Hair growth is slow—most plans need 3–6 months to judge improvement.
Some treatments can cause temporary increased shedding early (your dermatologist will explain if this applies).
Use gentle scalp care: mild shampoo, avoid harsh scrubs, minimize tight hairstyles.
Keep follow-up appointments so we can adjust the plan.
If you had a scalp biopsy
Keep the bandage on and dry for the first 24 hours (unless instructed otherwise).
- After 24 hours, daily:
Gently clean with mild soap and water
Pat dry
Apply a thin layer of ointment if instructed
Cover with a clean bandage
- Avoid swimming/hot tubs until cleared.
- Call if you have increasing redness, warmth, swelling, pus, fever, or bleeding that won’t stop with pressure.
When to Contact Us Urgently
Please contact us promptly if you have:
Painful, burning scalp with rapid hair loss
Pus, oozing, or spreading redness
Bald patches that are expanding quickly
Hair loss with new systemic symptoms (fever, severe fatigue)
Frequently Asked Questions
Is hair loss always permanent?
No. Many types (like telogen effluvium) are temporary. Others can be slowed or stabilized with the right treatment. Scarring alopecia is the main category where untreated inflammation can cause permanent loss.
How do I know if I’m shedding too much?
Seeing some hair daily is normal. If you notice a sudden increase in hair on your pillow, shower drain, or brush—or a noticeably thinner ponytail—an evaluation can help.
Why did my hair start shedding months after I was sick or stressed?
That timing is common with telogen effluvium—a trigger can shift more hairs into a resting phase, and shedding often begins 2–3 months later.
Do supplements help hair loss?
They help if you have a deficiency (like low iron), but supplements aren’t a cure-all. Taking high-dose supplements without guidance can be unnecessary or even harmful. We’ll recommend testing when appropriate.
Can hormones cause hair loss?
Yes. Hormones can influence pattern hair loss and shedding, especially around postpartum changes, menopause, or conditions like PCOS. Your dermatologist will consider this based on your history.
Is dandruff or scalp inflammation related to hair loss?
It can be. Inflammation and scratching can worsen shedding. Certain scalp conditions also mimic hair loss. Treating scalp health is often part of the plan.
Do I need blood work?
Sometimes. Labs can help identify treatable contributors like thyroid imbalance or iron deficiency. Not everyone needs the same tests—your clinician will tailor it to your case.
Do I need a scalp biopsy?
Only in certain situations—especially if we suspect scarring alopecia or the diagnosis isn’t clear from exam and history.
How long until I see regrowth?
Hair grows slowly. Meaningful change often takes 3–6 months, and fuller improvement may take longer depending on the cause and treatment.
