 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
- Acne & Acne Scarring
- Rosacea
Psoriasis (includes Excimer laser, Narrow band UVB phototherapy)
- Eczema (Atopic Dermatitis)
- Seborrheic Dermatitis
- Contact Dermatitis
- Hives (Urticaria)
- Vitiligo (includes Excimer laser, Narrow band UVB phototherapy)
- Hair Loss (Alopecia)
- Pruritus (Chronic Itching)
- Autoimmune Skin Disorders
- Warts, Molluscum, Fungal
- Sarcoidosis (Skin Involvement)
- Hyperhidrosis (Excessive Sweating)
- Lichen planus
- Blistering Skin Disorders
- Bacterial Skin Infections
- Keloids (Overgrown scar)
- Paraneoplastic Dermatoses (a clue to an internal cancer)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Psoriasis
What is psoriasis?
Psoriasis is a chronic (long-term), immune-mediated skin condition that causes skin cells to build up too quickly, leading to thick, inflamed patches (plaques) with scale. It is not contagious.
Many people have flares that come and go. With the right plan, psoriasis can be well controlled.
Types of psoriasis
You may have one type or a combination over time:
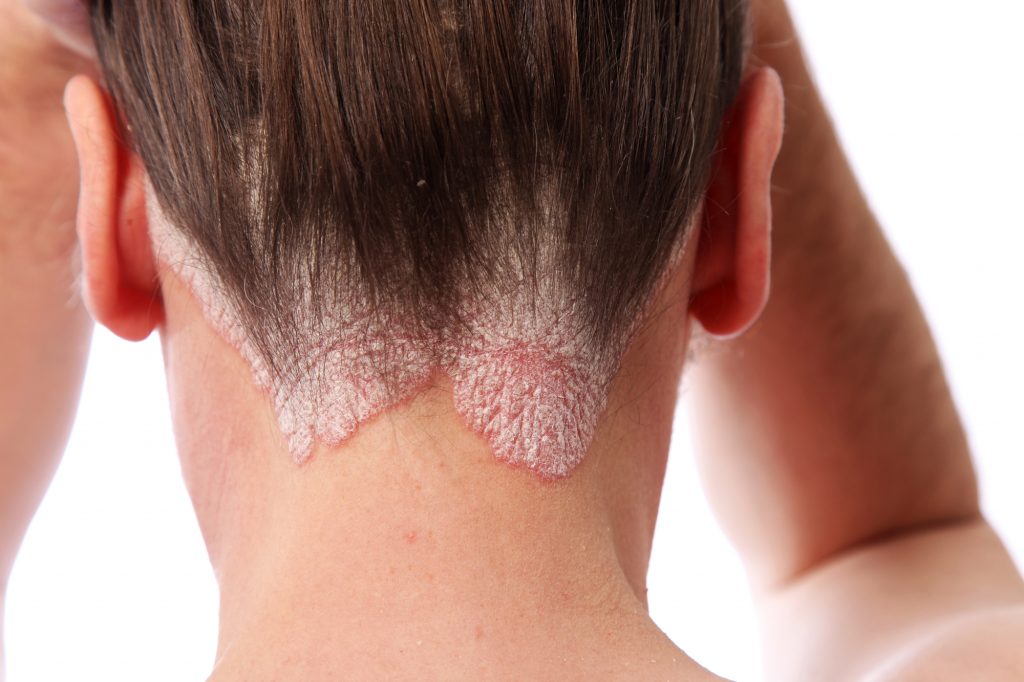
1) Plaque Psoriasis (Psoriasis Vulgaris)
Most common type of psoriasis
Appears as raised, red patches covered with thick silvery-white scale
Commonly affects the elbows, knees, scalp, and lower back
Can itch, crack, or bleed
Often chronic but very treatable with topical therapy, phototherapy, and systemic medications

2) Guttate psoriasis
Characterized by small, drop-shaped red spots
Often appears suddenly, especially in children or young adults
Commonly triggered by strep throat or other infections
Usually affects the trunk, arms, and legs
May resolve on its own or evolve into a) plaque psoriasis
3) Inverse psoriasis (skin folds)
Occurs in skin folds such as the armpits, groin, under the breasts, and buttocks
Appears smooth, red, and shiny (usually no thick scale)
Can be worsened by friction, sweating, and yeast infections
Often misdiagnosed as a fungal rash
4) Pustular psoriasis
Features white pus-filled bumps surrounded by red skin
Can be localized (hands and feet) or widespread
May be accompanied by fever or fatigue in severe cases
Less common but can be serious, requiring prompt medical care
5) Erythrodermic psoriasis
Rare but severe form of psoriasis
Causes widespread redness, intense scaling, and skin peeling
Can disrupt body temperature and fluid balance
Often triggered by infection, medication withdrawal, or severe sunburn
Considered a medical emergency
Why psoriasis happens
Psoriasis is related to immune system activity and genetics. Triggers can include:
Stress
Illness/infections
Skin injury (scratches, burns)
Certain medications
Cold/dry weather
How we diagnose psoriasis
Diagnosis is usually made with:
A focused history and skin exam
Sometimes dermoscopy or a skin biopsy if the diagnosis is unclear
Treatment options
Treatment is personalized based on the type, location, and severity.
1) At-home treatments (often first-line)
Prescription topical medications (creams/ointments)
Moisturizers and gentle skin-barrier care
2) In-office treatments
Narrow band UVB Phototherapy (light therapy) or Excimer Laser for widespread or stubborn psoriasis
3) For moderate-to-severe psoriasis
Oral or injectable medications, including biologics (when appropriate)
Why Light Therapy Helps Psoriasis
Phototherapy uses carefully measured ultraviolet light to:
Slow down overactive skin cell growth
Reduce inflammation and redness
Improve scaling and thickness of plaques
- Help control flares and extend periods of clear skin
Narrowband UVB (NB-UVB) Phototherapy
NB-UVB is one of the most common and effective in-office light treatments for psoriasis.
Best for:
Widespread plaque psoriasis (multiple areas)
Psoriasis that hasn’t responded enough to topical treatments
Patients who want a non-systemic option
What a typical course looks like:
Treatments are usually quick (often minutes)
Common schedule: 2–3 times per week for several weeks
Your dose is gradually increased to balance results and safety
NB-UVB vs Excimer:
Excimer laser delivers a targeted UVB wavelength to specific plaques, sparing surrounding normal skin.
Best for:
Localized psoriasis (small or stubborn areas)
Scalp edges, elbows, knees, or “few tough plaques”
Patients who want targeted treatment with fewer exposures to uninvolved skin
What a typical course looks like:
Usually 1–2 times per week
Often fewer sessions for small areas (varies by plaque thickness and response)
NB-UVB vs Excimer: Which One Do I Need?
Choose NB-UVB if psoriasis is more widespread
Choose Excimer if psoriasis is localized or stubborn
Many patients benefit from a combined plan (topicals + phototherapy)
Your dermatologist will recommend the best approach based on your psoriasis pattern, skin type, lifestyle, and prior treatments.
Pre-Op Instructions (Before Phototherapy)
(No fasting is needed. These are “before-treatment” tips.)
1–2 weeks before starting
Avoid tanning and sunburn
Tell us if you:
Take medications that increase sun sensitivity (some antibiotics, diuretics, etc.)
Have a history of frequent cold sores (for facial treatment planning)
Have a history of skin cancer or photosensitivity disorders
Let us know if you are pregnant or trying to conceive (treatment planning may change)
Day of treatment
Arrive with clean, dry skin on treatment areas
Avoid perfumes, body oils, or heavy lotions on areas being treated (unless we tell you otherwise)
Bring or use protective eyewear as directed (we provide guidance)
Wear easy clothing to access the treatment areas
Post-Op Instructions (After NB-UVB or Excimer Treatments)
What’s normal after treatment
Mild redness or warmth (similar to a mild sun exposure)
Mild itching or dryness
Gradual smoothing and fading of plaques over weeks
Skin care after sessions
Moisturize daily with a gentle, fragrance-free moisturizer
Use gentle cleanser; avoid harsh scrubs/exfoliants on treated areas
Use sun protection (hat, protective clothing, sunscreen as appropriate)
Activity tips
You can usually return to normal activities right away
Avoid intentional sun exposure or tanning while undergoing treatment
Call our office if you have:
A painful burn, blistering, or significant swelling
Increasing redness that continues to worsen after 24–48 hours
New rash in areas not being treated
Frequently Asked Questions
Is psoriasis contagious?
No. Psoriasis is not contagious.
Is psoriasis curable?
Psoriasis is chronic, meaning it often requires long-term management, but it can usually be well controlled with the right plan.
How long does treatment take to work?
Many treatments take weeks to show major improvement. Your plan may be adjusted over time based on response.
What’s the difference between psoriasis and eczema?
Both can itch and cause inflammation, but psoriasis often forms thicker plaques with scale, while eczema commonly causes more diffuse, very itchy inflammation. A dermatologist can confirm the diagnosis.
Can psoriasis affect my nails?
Yes. Psoriasis can cause nail pitting, discoloration, thickening, or lifting.
Can psoriasis affect joints?
Yes. Some people develop psoriatic arthritis, which can cause joint pain, swelling, and stiffness. Tell us if you have these symptoms so we can coordinate care.
What can I do at home to reduce flares?
Moisturize daily
Use gentle, fragrance-free skincare
Manage stress and get adequate sleep
Avoid triggers you notice (illness, skin injury, harsh products)
Use sun protection (avoid sunburn)
When should I schedule an appointment?
If you have a persistent scaly rash, symptoms that affect sleep or daily life, nail changes, or any joint symptoms, an evaluation can help you get the right diagnosis and treatment plan.
Is phototherapy safe?
When supervised and dosed correctly, Narrow Band-UVB and Excimer Laser are widely used and considered safe. Your dermatologist monitors dosing to reduce burn risk.
Will phototherapy hurt?
Treatments are typically painless. Some patients feel warmth during treatment or mild redness afterward.
Will I get burned with phototherapy?
A mild, short-lived pinkness can be expected. A true burn is uncommon but can happen—especially if you’ve had sun exposure or started a sun-sensitizing medication. Tell us about medication changes and sun exposure.
Can I do phototherapy if I have psoriasis on my scalp?
Yes. Both NB-UVB (with proper scalp access strategies) and excimer can be used for scalp-adjacent or localized plaques. Your dermatologist will recommend what fits best.
Can phototherapy help itch?
Yes—many patients experience reduced itch as inflammation improves.
Do I still need topical medications with phototherapy treatment?
Often yes. Phototherapy works very well with a supportive topical routine. Your dermatologist will guide a safe combination plan.
