 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
- Acne & Acne Scarring
- Rosacea
- Psoriasis (includes Excimer laser, Narrow band UVB phototherapy)
- Eczema (Atopic Dermatitis)
- Seborrheic Dermatitis
- Contact Dermatitis
- Hives (Urticaria)
Vitiligo (includes Excimer laser, Narrow band UVB phototherapy)
- Hair Loss (Alopecia)
- Pruritus (Chronic Itching)
- Autoimmune Skin Disorders
- Warts, Molluscum, Fungal
- Sarcoidosis (Skin Involvement)
- Hyperhidrosis (Excessive Sweating)
- Lichen planus
- Blistering Skin Disorders
- Bacterial Skin Infections
- Keloids (Overgrown scar)
- Paraneoplastic Dermatoses (a clue to an internal cancer)
- Skin Issues Related to STDs (STIs)
- Scabies
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Vitiligo
(Loss of skin pigment that causes white patches)
What Is Vitiligo?
Vitiligo is a condition where areas of skin lose pigment (color), leading to white or lighter patches. It can affect any part of the body, and it can also affect hair (turning it white) and sometimes the inside of the mouth. Vitiligo is not contagious.
Vitiligo often has periods of change and stability. Some people choose not to treat it, while others want treatment to restore pigment and/or slow progression—both are valid choices.

What Does Vitiligo Look Like?
Vitiligo commonly appears as:
Smooth white or lighter patches
Sharply defined borders
Common areas: face, hands, arms, feet, and around body openings (mouth/eyes)
How We Diagnose Vitiligo
Diagnosis is usually made with:
A focused history and skin exam
Sometimes a special light exam in the office to help define pigment loss
Rarely, additional testing if another condition needs to be ruled out
Vitiligo Treatment Options
Your plan depends on patch location, how widespread vitiligo is, and whether it’s active.
1) Topical medications (creams/ointments)
These can help calm inflammation and support repigmentation in selected areas, especially on the face.
2) Narrowband UVB (NB-UVB) phototherapy
NB-UVB is a common, effective option for more widespread vitiligo. Treatment is typically done 2–3 times per week, and results usually take time—often months, not days.
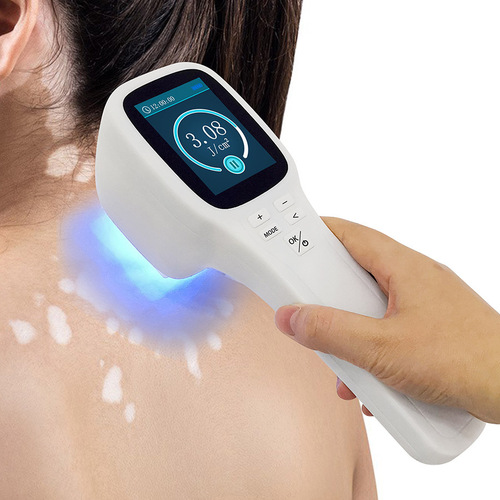
3) Excimer light/laser (308 nm)
Excimer is targeted light therapy—great for smaller, localized patches because it treats the spots while sparing unaffected skin.
4) Combination plans
Many patients do best with a combined approach (for example: topical therapy + phototherapy), depending on goals and skin type.
Pre-Op Instructions (Before Phototherapy or Excimer)
(No fasting needed — these are “before treatment” tips.)
1–2 weeks before starting
Avoid tanning and sunburn
Tell us if you:
Take medications that increase sun sensitivity
Have a history of frequent skin cancers or photosensitivity disorders
Are pregnant or trying to conceive (we’ll tailor options)
Day of treatment
Arrive with clean, dry skin on treatment areas
Avoid perfumes/body oils on treated areas (unless we instruct otherwise)
Bring a list of all medications and topical products you use
Post-Op Instructions (After Phototherapy or Excimer)
a) What’s normal
Mild pinkness/warmth for a few hours
Mild dryness or itch
Gradual, patchy repigmentation over time (often first seen as tiny “freckles” of color)
Skin care after sessions
Use a gentle moisturizer daily
Avoid hot showers/saunas/exercise that overheats you for 24 hours if you tend to get red easily
Use consistent sun protection (vitiligo patches burn more easily)
Call our office if you have
Painful redness like a sunburn that lasts >24–48 hours
Blistering, significant swelling, or worsening discomfort
New rash outside treatment areas
Frequently Asked Questions
Is vitiligo dangerous?
Vitiligo isn’t usually physically dangerous, but it can increase sun sensitivity in the lighter patches, and it can significantly affect confidence and quality of life.
Is vitiligo contagious?
No—vitiligo is not contagious.
What’s the best treatment: NB-UVB or excimer?
NB-UVB is often used for widespread vitiligo.
Excimer (308 nm) is often used for localized patches.
Your dermatologist will recommend the best fit for your pattern and schedule.
How long does it take to see results?
Many patients need multiple weeks to months to notice pigment returning, and longer courses may improve response.
Can vitiligo spread?
It can. Narrow Band-UVB phototherapy has been shown to help slow progression in active vitiligo.
Will vitiligo come back after treatment?
It can. Some people need maintenance strategies and ongoing follow-up.
Is there a prescription cream specifically approved for vitiligo?
Yes. Opzelura® (ruxolitinib) cream is FDA-approved for nonsegmental vitiligo in ages 12+.
Should I use sunscreen on vitiligo patches?
Yes—lighter patches are more likely to burn. Daily broad-spectrum sunscreen and sun-protective clothing are strongly recommended.
