 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
- Acne & Acne Scarring
- Rosacea
- Psoriasis (includes Excimer laser, Narrow band UVB phototherapy)
Eczema (Atopic Dermatitis)
- Seborrheic Dermatitis
- Contact Dermatitis
- Hives (Urticaria)
- Vitiligo (includes Excimer laser, Narrow band UVB phototherapy)
- Hair Loss (Alopecia)
- Pruritus (Chronic Itching)
- Autoimmune Skin Disorders
- Warts, Molluscum, Fungal
- Sarcoidosis (Skin Involvement)
- Hyperhidrosis (Excessive Sweating)
- Lichen planus
- Blistering Skin Disorders
- Bacterial Skin Infections
- Keloids (Overgrown scar)
- Paraneoplastic Dermatoses (a clue to an internal cancer)
- Skin Issues Related to STDs (STIs)
- Scabies
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Eczema (Atopic Dermatitis)
1. What Is Eczema (Atopic Dermatitis)?
Eczema, also called atopic dermatitis, is a common, long-term inflammatory skin condition that causes dry, itchy, sensitive skin and sometimes red, rough, or scaly patches. It tends to flare and improve over time (a “relapsing” pattern).
Eczema is not contagious—you cannot “catch” it from someone else.
2. What Does Eczema Look Like?
Eczema can look different by age, skin tone, and body location. Common features include:
Itching (sometimes intense)
Dryness and rough texture
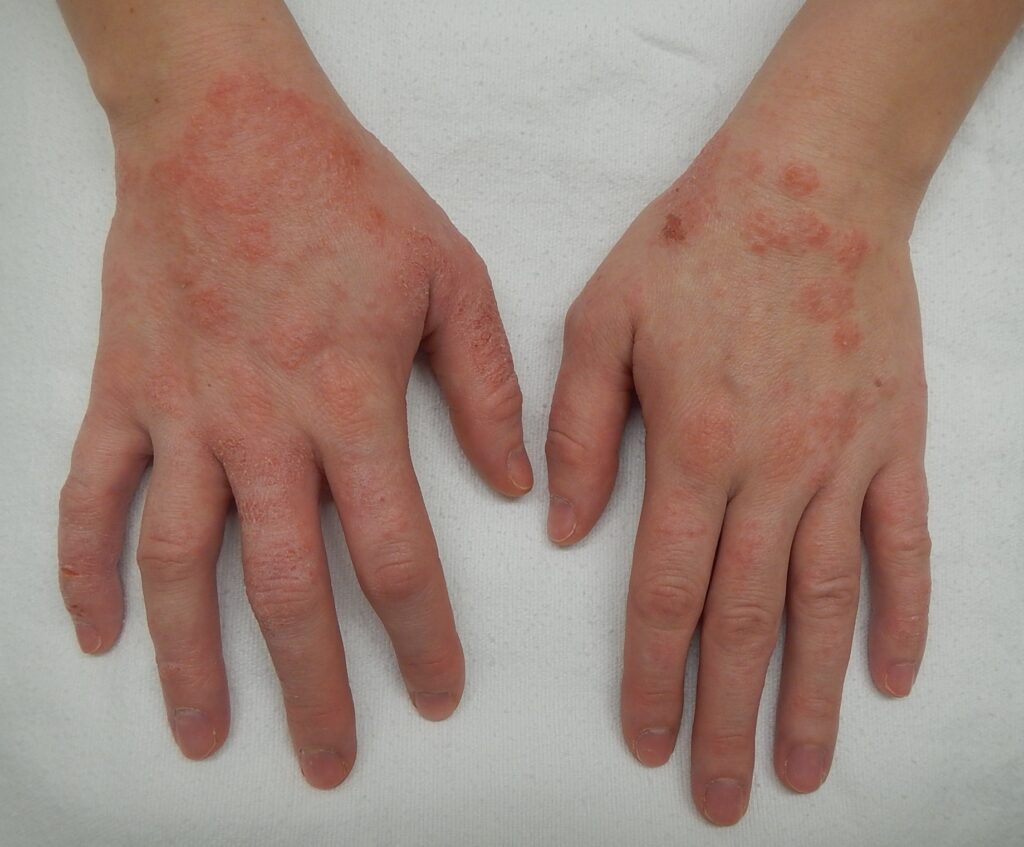
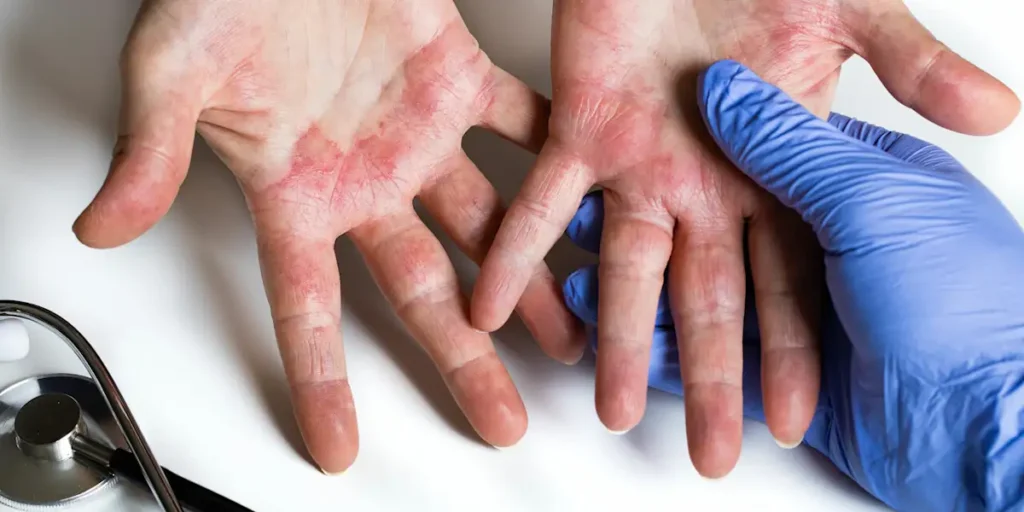
Redness or darker/lighter discoloration (varies by skin tone)
Scaling, cracking, or thickened skin from chronic rubbing/scratching
Sometimes oozing/crusting during flares
Common locations:
Children: cheeks, arms/legs, skin folds
Adults: hands, wrists, eyelids, neck, skin folds; can be widespread
3. Why Eczema Happens
Eczema is often related to a combination of:
Skin barrier weakness (skin loses moisture easily and becomes sensitive)
Immune system inflammation
Genetics and a tendency toward allergies/asthma in some families
4. Common Triggers
Many people notice flares with:
Dry/cold weather
Heat, sweating
Fragrances or harsh soaps
Frequent handwashing / sanitizers (hand eczema)
Stress, illness
Certain fabrics (wool) or detergents
Identifying triggers helps reduce flare frequency.
5. How We Diagnose Eczema
Diagnosis is usually based on:
Your history (itch pattern, triggers, family history)
Skin exam
In some cases: patch testing (if allergic contact dermatitis is suspected) or a skin biopsy if the diagnosis is unclear
6. Treatment Options
Your plan depends on severity, location, age, and flare pattern.
a) Daily Skin Barrier Care (Foundation of Treatment)
Gentle, fragrance-free cleanser
Short, lukewarm showers
Moisturize at least 1–2 times daily (especially after bathing)
b) Prescription Topical Medications (Flares)
Anti-inflammatory creams/ointments to calm itching and redness
Steroid-sparing options for sensitive areas (face/eyelids/skin folds) when appropriate
c) Treatments for Moderate-to-Severe Eczema
If eczema is widespread, frequently flaring, or affecting sleep and quality of life, options may include:
Phototherapy (light therapy)
Oral or injectable anti-inflammatory medications (selected patients)
Targeted therapies when appropriate (your dermatologist will guide what’s safest for you)
d) Treating Infection (When Present)
Eczema skin can be more prone to infection. If we suspect infection, we may recommend specific treatments and updated skin-care steps.
7. Pre-Op Instructions (Before Your Eczema Visit or Procedure)
(Most eczema care is not “surgery,” but these tips help you get the best results.)
a) Before your evaluation
Bring a list of current products (soap, shampoo, moisturizer, “natural” products)
Note what triggers flares and where it occurs
Tell us if you have asthma, allergies, or frequent skin infections
b) If you’re scheduled for patch testing
Ask us which medications to avoid beforehand (some can interfere with results)
Avoid applying creams to the test area as instructed
c) If phototherapy is scheduled
Avoid tanning/sunburn before sessions
Tell us about any sun-sensitizing medications
8. Post-Op Instructions (After Starting Treatment)
a) After starting prescription creams
Use exactly as directed (overuse and underuse can both cause problems)
Expect improvement over days to weeks, depending on severity
Continue moisturizer daily even when the flare improves
b) After phototherapy (if used)
Mild pinkness can happen
Moisturize daily
Avoid extra sun exposure the same day unless your dermatologist advises otherwise
c) Call our office promptly if you notice
Rapidly worsening redness, pain, warmth, swelling, or pus
Fever, chills, or feeling unwell
Painful clusters of blisters (especially on the face)—this needs urgent evaluation
Frequently Asked Questions
Is eczema the same as dry skin?
Dry skin can be part of eczema, but eczema also includes inflammation and itch and often needs targeted treatment during flares.
Is eczema contagious?
No—eczema is not contagious.
Why does eczema itch so much?
Eczema affects the skin barrier and triggers inflammation that makes the skin extra sensitive and itchy. Scratching can worsen the barrier and keep the itch cycle going.
Can eczema happen on the hands only?
Yes—hand eczema is common and may be triggered by frequent washing, sanitizers, or irritants at work or home.
What’s the best moisturizer for eczema?
In general, choose fragrance-free, thick creams or ointments. We can recommend options based on whether your eczema is on the face, body, or hands.
Do I need allergy testing for eczema?
Not always. If we suspect your rash is being driven by an allergic contact trigger (like fragrances, preservatives, metals, or topical products), patch testing may help.
Can diet cause eczema?
Some people notice food-related flares, especially children, but it’s not the main driver for most patients. We focus on evidence-based steps and only recommend dietary changes when clearly appropriate.
When should I see a dermatologist?
If eczema is affecting sleep, spreading, frequently infected, not improving with Over-the-counter (OTC) care, or causing significant discomfort—professional care can make a big difference.
