 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
- Acne & Acne Scarring
- Rosacea
- Psoriasis (includes Excimer laser, Narrow band UVB phototherapy)
- Eczema (Atopic Dermatitis)
- Seborrheic Dermatitis
- Contact Dermatitis
- Hives (Urticaria)
- Vitiligo (includes Excimer laser, Narrow band UVB phototherapy)
- Hair Loss (Alopecia)
- Pruritus (Chronic Itching)
- Autoimmune Skin Disorders
- Warts, Molluscum, Fungal
- Sarcoidosis (Skin Involvement)
- Hyperhidrosis (Excessive Sweating)
- Lichen planus
- Blistering Skin Disorders
- Bacterial Skin Infections
- Keloids (Overgrown scar)
Paraneoplastic Dermatoses (a clue to an internal cancer)
- Skin Issues Related to STDs (STIs)
- Scabies
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Paraneoplastic Dermatoses
Skin changes that can (rarely) be a clue to an internal cancer
What Are Paraneoplastic Dermatoses?
Paraneoplastic dermatoses are unusual skin findings linked to an underlying cancer, but the skin problem itself is not cancer spreading to the skin. Instead, the skin reacts to signals from the tumor or the immune system. These skin changes may appear before, at the same time as, or after a cancer diagnosis.
Most rashes and growths are not paraneoplastic. But when certain skin patterns appear suddenly or behave unusually, they can serve as a “red flag” that prompts further evaluation.
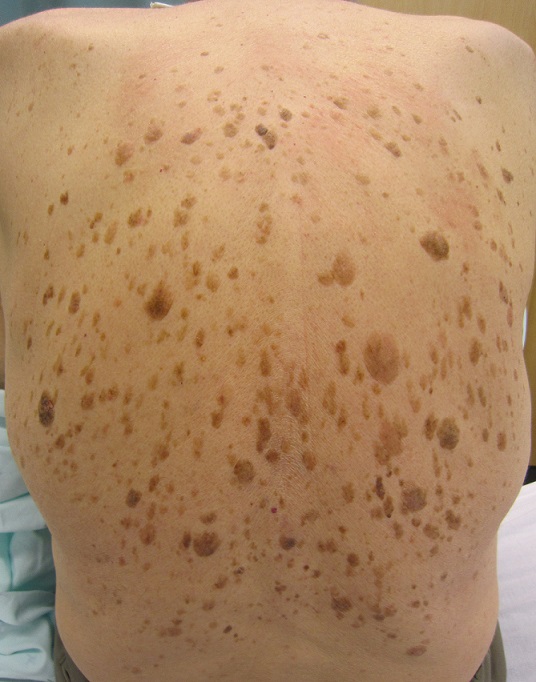
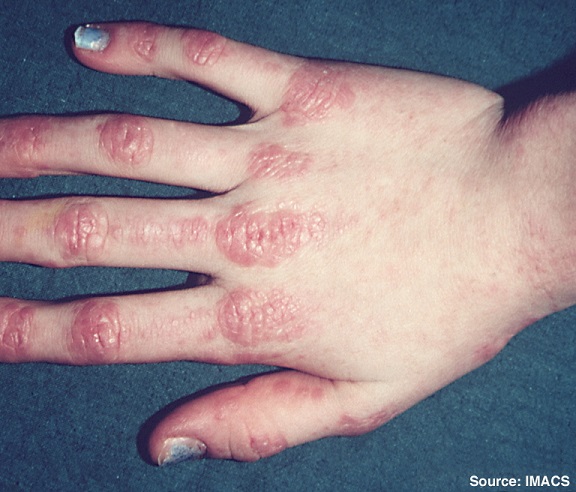
Common Examples We Watch For
Your dermatologist may consider a paraneoplastic cause when skin findings have a classic look and new, rapid onset, especially with other symptoms (weight loss, fatigue, fevers, night sweats).
Examples include:
Acanthosis nigricans (sudden onset): velvety dark thickening, often on neck/armpits
Dermatomyositis: rash with muscle weakness (can be associated with internal malignancy in adults)
Sign of Leser-Trélat: sudden eruption of many “stuck-on” growths (seborrheic keratoses)
Erythema gyratum repens: rapidly spreading “wood-grain” patterned rash (rare)
Paraneoplastic pruritus: persistent, unexplained itching (a possible internal marker in some cases)
Symptoms That Should Prompt an Evaluation
Call our office for assessment if you notice:
A new rash that spreads quickly or doesn’t respond to usual treatment
Sudden onset of many new growths or rapidly changing skin findings
Unexplained itching that is severe or persistent
Skin changes plus systemic symptoms like unintentional weight loss, fevers, night sweats, fatigue, or new lumps
Seek urgent care if you have blistering/peeling skin, facial swelling, trouble breathing, or rapidly worsening illness.
How We Evaluate Paraneoplastic Dermatoses
Because many of these findings can mimic common skin conditions, evaluation is step-by-step:
History & full skin exam (timing, symptoms, medications, family history)
Skin biopsy (often the most helpful next step)
Targeted labs (if indicated)
Coordinate age-appropriate cancer screening with your PCP
If concern remains: referral coordination (oncology, GI, gynecology, etc.)
If cancer screening is needed, we help guide what to do next, but the specific work-up is individualized.
Pre-Op Instructions (If a Skin Biopsy Is Planned)
Most patients don’t need special preparation, but these steps help procedures go smoothly:
Tell us if you take blood thinners or have a bleeding disorder
⚠️ Do not stop prescription blood thinners unless the prescribing clinician instructs you.Arrive with clean skin (avoid heavy lotions/oils on the area)
Let us know about allergies (tape/adhesives, antiseptics, numbing medicine)
If the site is hairy (scalp/arm/leg), don’t shave right before—small nicks can irritate skin
Post-Op Instructions (After Biopsy)
Keep the bandage on and dry for 24 hours (unless instructed otherwise)
Then: gentle wash with soap/water, pat dry, apply a thin layer of ointment if directed, and cover with a clean bandage
Avoid soaking (pools/hot tubs/baths) until healed
Call us if you notice worsening redness, warmth, swelling, pus-like drainage, fever, or bleeding that won’t stop after 10–15 minutes of firm pressure
Frequently Asked Questions
Is a paraneoplastic rash the same as skin cancer?
No. Paraneoplastic dermatoses are skin reactions associated with an internal cancer, not cancer cells growing in the skin.
Does having one of these rashes mean I have cancer?
Not necessarily. Many of these skin findings have benign causes. The key is the pattern, sudden onset, and overall clinical picture.
Why would cancer affect the skin?
Some cancers trigger immune responses or release signals that can cause skin changes—even when the cancer is located elsewhere.
How do you confirm the diagnosis?
A skin biopsy is often the most helpful test. Depending on the results, we may recommend labs and coordination with your primary care clinician for additional screening.
If cancer is found and treated, will the skin improve?
Often, paraneoplastic skin findings improve when the underlying cancer is treated, though this varies by condition and individual.
What is “paraneoplastic pruritus”?
It’s persistent, unexplained itching that can sometimes be associated with internal disease. Itching has many common causes, so evaluation helps rule out more serious conditions.
When should I be worried?
If you have a rapidly spreading rash, new blisters/skin peeling, or skin changes plus systemic symptoms (fever, weight loss, night sweats), contact us promptly.
