 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
- Acne & Acne Scarring
- Rosacea
- Psoriasis (includes Excimer laser, Narrow band UVB phototherapy)
- Eczema (Atopic Dermatitis)
- Seborrheic Dermatitis
- Contact Dermatitis
- Hives (Urticaria)
- Vitiligo (includes Excimer laser, Narrow band UVB phototherapy)
- Hair Loss (Alopecia)
- Pruritus (Chronic Itching)
- Autoimmune Skin Disorders
- Warts, Molluscum, Fungal
- Sarcoidosis (Skin Involvement)
- Hyperhidrosis (Excessive Sweating)
Lichen planus
- Blistering Skin Disorders
- Bacterial Skin Infections
- Keloids (Overgrown scar)
- Paraneoplastic Dermatoses (a clue to an internal cancer)
- Skin Issues Related to STDs (STIs)
- Scabies
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Lichen planus
A chronic inflammatory skin condition affecting skin, mouth, scalp, or nails
What Is Lichen Planus?
Lichen planus is an inflammatory condition that can affect the skin, mouth (oral mucosa), scalp, nails, or genital area. It is believed to be immune-mediated, meaning the immune system triggers inflammation in the skin or mucous membranes.
It is not contagious and is not caused by poor hygiene.
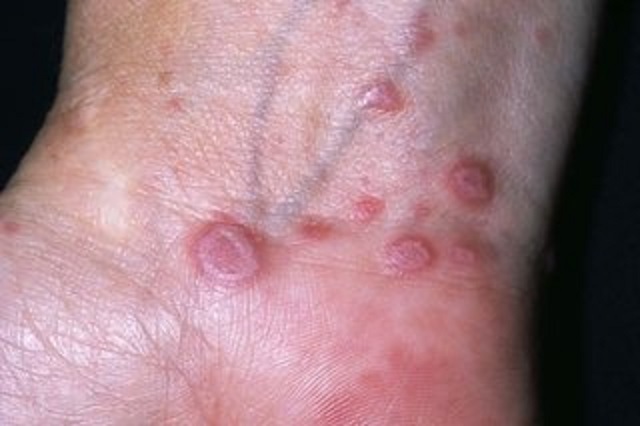
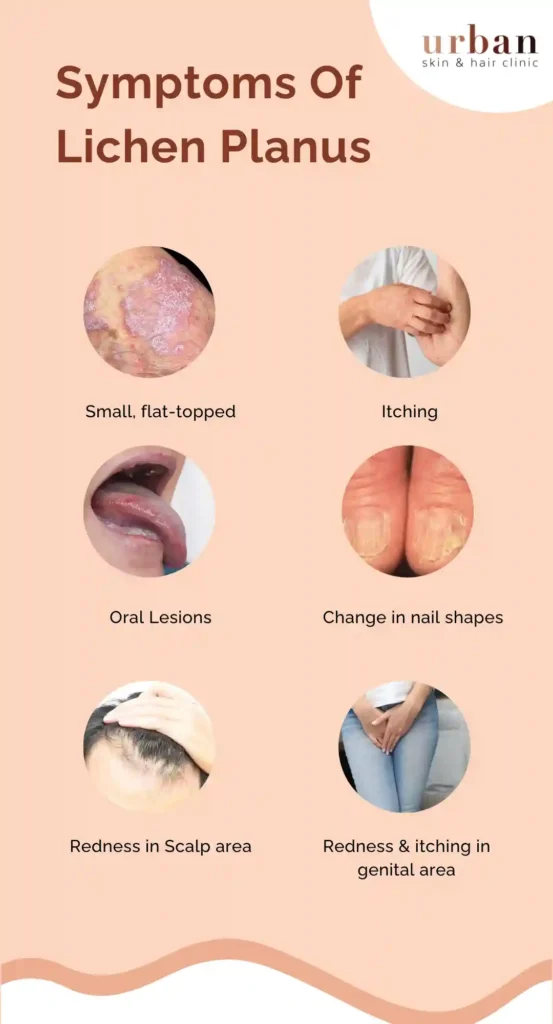
What Does Lichen Planus Look Like?
On the Skin
Small, flat-topped purple or reddish bumps
Often itchy
Common on wrists, ankles, lower legs, or lower back
May leave dark marks (post-inflammatory hyperpigmentation) after healing
In the Mouth (Oral Lichen Planus)
White, lace-like patches inside cheeks
Red or irritated areas
Possible sensitivity to spicy or acidic foods
On the Scalp (Lichen Planopilaris)
Redness or scaling
Hair thinning or permanent hair loss if untreated
On Nails
Ridging or thinning
Nail splitting
Rarely, nail loss
On Genital Area
Redness and itching
What Causes Lichen Planus?
The exact cause is unknown. Possible triggers include:
Immune system overactivity
Certain medications
Viral infections (in some cases)
Stress (may worsen symptoms)
Your dermatologist may recommend evaluation or testing depending on the presentation.
How Is Lichen Planus Treated?
Treatment depends on the severity and location.
Common treatment options include:
Topical corticosteroids (first-line for many patients)
Topical calcineurin inhibitors
Oral medications (for widespread or severe cases)
Steroid injections (for localized lesions)
Phototherapy (in selected patients)
For oral or scalp involvement, treatment is tailored carefully to prevent complications.
Is Lichen Planus Permanent?
Skin lichen planus may resolve within months to a few years
Oral lichen planus can be chronic
Scalp involvement requires early treatment to prevent permanent hair loss
Ongoing monitoring may be recommended.
Pre-Op Instructions (If Biopsy or Procedure Is Needed)
Most lichen planus is diagnosed clinically, but a skin biopsy may sometimes be needed.
If biopsy is planned:
Continue regular medications unless instructed otherwise
Inform us if you take blood thinners
Arrive with clean skin
Follow standard minor procedure instructions
Post-Op Instructions (After Biopsy or Injections)
What’s Normal:
Mild soreness or redness
Small scab at biopsy site
Temporary bruising (after injections)
Aftercare:
Keep the area clean and dry
Apply ointment as directed
Avoid picking or scratching
Follow wound care instructions carefully
Call the office if:
You develop increasing pain, swelling, or drainage
The area does not heal as expected
Frequently Asked Questions
Is lichen planus contagious?
No. It cannot be spread to others.
Is it an autoimmune disease?
It is considered immune-mediated, meaning the immune system plays a role in triggering inflammation.
Does lichen planus cause permanent damage?
- Skin lesions often resolve but may leave temporary dark marks.
- Scalp involvement (lichen planopilaris) can cause permanent hair loss if not treated early.
Is oral lichen planus serious?
Oral lichen planus is usually manageable but should be monitored. In rare cases, long-term changes may require closer follow-up.
Does stress make it worse?
Stress may worsen inflammation in some patients.
Can lichen planus come back?
Yes. It may flare or improve over time.
Is lichen planus related to cancer?
- Skin lichen planus is not cancer.
- Oral lichen planus requires periodic monitoring because chronic irritation can rarely lead to changes over many years.
