 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
- Acne & Acne Scarring
- Rosacea
- Psoriasis (includes Excimer laser, Narrow band UVB phototherapy)
- Eczema (Atopic Dermatitis)
- Seborrheic Dermatitis
- Contact Dermatitis
- Hives (Urticaria)
- Vitiligo (includes Excimer laser, Narrow band UVB phototherapy)
- Hair Loss (Alopecia)
- Pruritus (Chronic Itching)
- Autoimmune Skin Disorders
- Warts, Molluscum, Fungal
Sarcoidosis (Skin Involvement)
- Hyperhidrosis (Excessive Sweating)
- Lichen planus
- Blistering Skin Disorders
- Bacterial Skin Infections
- Keloids (Overgrown scar)
- Paraneoplastic Dermatoses (a clue to an internal cancer)
- Skin Issues Related to STDs (STIs)
- Scabies
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Sarcoidosis (Skin Involvement)
(An inflammatory condition that can affect the skin and other organs)
1. What Is Sarcoidosis?
Sarcoidosis is an inflammatory condition in which the immune system forms small clusters of inflammatory cells, called granulomas, in different parts of the body. It can affect many organs—most commonly the lungs and lymph nodes—and it can also involve the skin.
Sarcoidosis is not contagious and not caused by infection. Its course varies widely: some people have mild disease that improves on its own, while others need ongoing treatment.
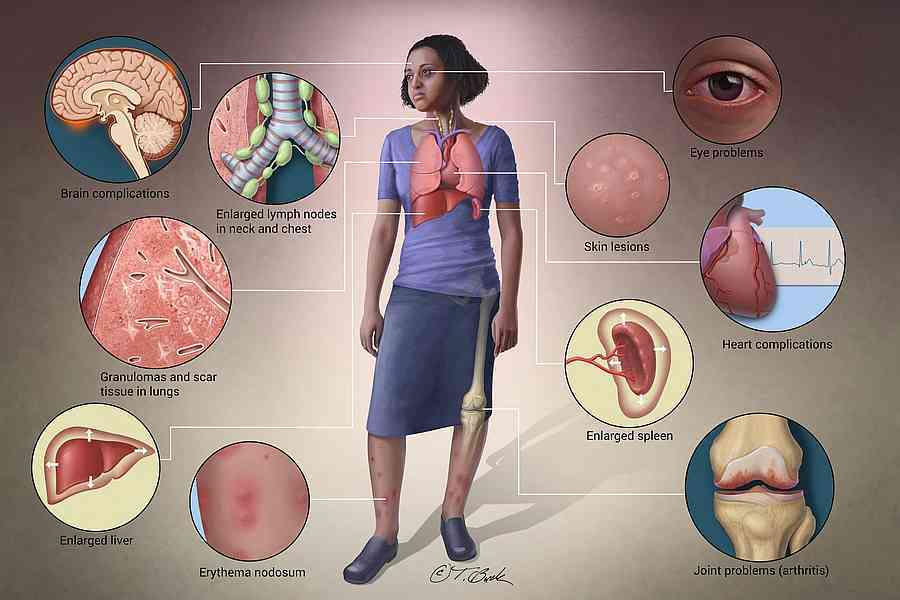
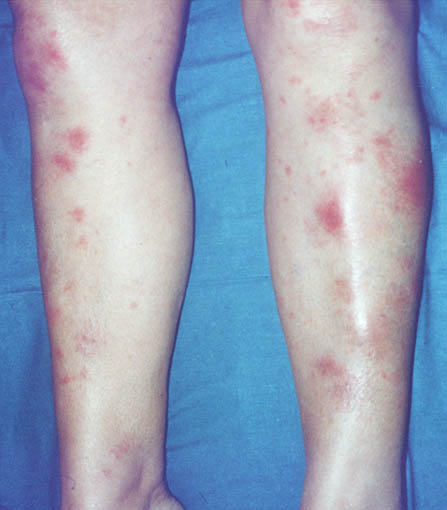
How Sarcoidosis Affects the Skin
Skin involvement (called cutaneous sarcoidosis) may be the first sign of sarcoidosis—or occur in people who already have a diagnosis.
Skin findings can include:
Firm bumps or plaques (skin-colored, red-brown, or purple)
Lesions on the face, neck, arms, or legs
Lupus pernio: violaceous thickening on the nose, cheeks, lips, or ears
Scars or tattoos that become raised or inflamed
Areas that don’t itch much but feel firm or tender
Because sarcoidosis skin lesions can look like many other conditions, evaluation by a dermatologist is important.
Other Symptoms to Mention
Even if you’re seeing us for skin changes, tell us if you also have:
Shortness of breath or persistent cough
Fatigue or unexplained weight loss
Joint pain or swelling
Eye irritation or vision changes
Enlarged lymph nodes
These details help guide testing and coordination of care.
How We Diagnose Sarcoidosis
Diagnosis often involves several steps:
1. Skin Examination
We look at lesion type, location, color, and firmness.
2. Skin Biopsy (Key Step)
A small sample of skin is removed and examined under the microscope. Sarcoidosis typically shows noncaseating granulomas.
This helps confirm the diagnosis and rule out look-alike conditions.
3. Additional Testing (When Needed)
If sarcoidosis is confirmed or suspected, we may coordinate:
Blood tests
Imaging (such as chest imaging)
Referrals to pulmonology, rheumatology, or ophthalmology
Treatment Options
Treatment depends on:
Severity of skin involvement
Symptoms
Whether other organs are affected
Skin-Directed Treatment
For limited skin disease:
Prescription topical medications to reduce inflammation
Local treatments for symptomatic or cosmetically sensitive areas
Systemic Treatment
If skin disease is extensive or other organs are involved:
Oral or injectable medications that calm the immune system
Coordinated care with other specialists
Some skin lesions may improve slowly—even with treatment—so patience and follow-up are important.
Pre-Op Instructions
(Not surgery—these are “before your visit or biopsy” tips)
Before Your Appointment
Take photos of skin lesions if they change or fade between visits
Bring a list of:
All medications and supplements
Any prior sarcoidosis testing or diagnoses
- Note any systemic symptoms (lungs, eyes, joints, fatigue)
If a Skin Biopsy Is Planned
Tell us if you:
Take blood thinners
Bruise easily
Have allergies to numbing medicine, antiseptics, or adhesives
⚠️ Do not stop prescribed blood thinners unless directed by your prescribing clinician.
Post-Op Instructions
After a Skin Biopsy
Keep the bandage on and dry for 24 hours (unless told otherwise)
After 24 hours, daily:
Clean gently with soap and water
Pat dry
Apply a thin layer of ointment if instructed
Cover with a clean bandage
Avoid soaking (baths, pools, hot tubs) until healed
Call if you notice increasing redness, warmth, swelling, pus, fever, or bleeding that won’t stop with pressure
After Starting Treatment
Use medications exactly as prescribed
Improvement may take weeks to months
Keep follow-up appointments so we can adjust your plan as needed
When to Seek Urgent Care
Seek urgent or emergency care if you develop:
Worsening shortness of breath or chest pain
Vision changes or severe eye pain
Neurologic symptoms (weakness, numbness, severe headache)
Rapidly worsening skin pain or blistering
Frequently Asked Questions
Is sarcoidosis contagious?
No. Sarcoidosis is not contagious.
Does sarcoidosis only affect the skin?
No. While some people have skin-limited disease, sarcoidosis can also affect the lungs, lymph nodes, eyes, joints, heart, or nervous system. That’s why coordination of care is important.
Is sarcoidosis an autoimmune disease?
It’s considered an immune-mediated inflammatory condition. The exact cause is unknown.
Why is a skin biopsy important?
Many rashes look similar. A biopsy helps confirm sarcoidosis and rule out infections or other inflammatory conditions that require different treatment.
Will sarcoidosis go away?
In some people, sarcoidosis improves or resolves over time. In others, it may be chronic and need ongoing management. The course is highly individual.
Does sun exposure affect sarcoidosis?
Sun sensitivity varies. Some skin lesions may darken or become more noticeable with sun exposure. We’ll advise you on sun protection based on your presentation.
Will sarcoidosis leave scars?
Some skin lesions may resolve without scarring, while others—especially thicker plaques—can leave texture or color changes.
How often will I need follow-up?
Follow-up depends on severity and whether other organs are involved. Your dermatologist will recommend an appropriate schedule.
