 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
- Acne & Acne Scarring
- Rosacea
- Psoriasis (includes Excimer laser, Narrow band UVB phototherapy)
- Eczema (Atopic Dermatitis)
- Seborrheic Dermatitis
- Contact Dermatitis
- Hives (Urticaria)
- Vitiligo (includes Excimer laser, Narrow band UVB phototherapy)
- Hair Loss (Alopecia)
- Pruritus (Chronic Itching)
- Autoimmune Skin Disorders
Warts, Molluscum, Fungal
- Sarcoidosis (Skin Involvement)
- Hyperhidrosis (Excessive Sweating)
- Lichen planus
- Blistering Skin Disorders
- Bacterial Skin Infections
- Keloids (Overgrown scar)
- Paraneoplastic Dermatoses (a clue to an internal cancer)
- Skin Issues Related to STDs (STIs)
- Scabies
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Warts, Molluscum & Fungal Infections
(Common contagious skin conditions we diagnose and treat)
Overview
Skin infections are very common—especially in children, athletes, and anyone with close skin-to-skin contact. Three frequent causes we treat are:
Warts (caused by certain types of HPV)
Molluscum contagiosum (a common poxvirus infection)
Fungal infections (like ringworm/tinea, athlete’s foot, and jock itch)
These conditions are usually treatable and often improve faster with the right diagnosis and plan.
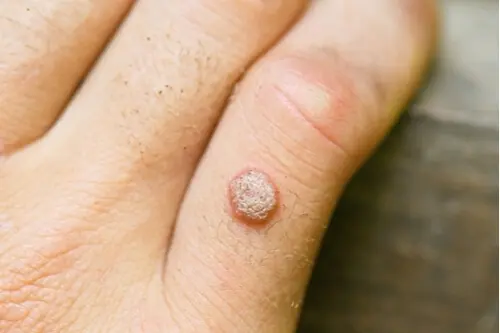
1. Warts
What are they?
Warts are rough, thickened bumps caused by a virus that infects the top layer of skin.
Common types
Common warts (hands/fingers)
Plantar warts (feet—can feel like stepping on a pebble)
Flat warts (small, smooth—often face/arms/legs)
Genital warts (treated differently—please ask for a dedicated visit)
How they spread
By direct contact or shared surfaces (gym floors, towels). Small skin breaks make it easier for the virus to enter.
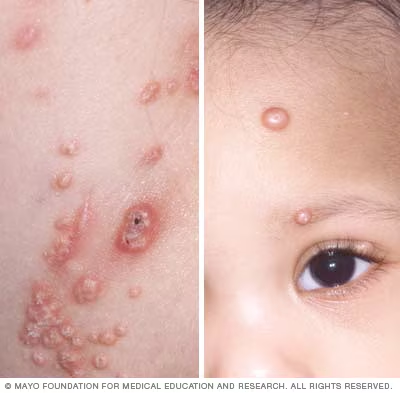
2. Molluscum Contagiosum
What is it?
Molluscum causes small, smooth, pearly bumps—often with a tiny central dimple. It’s common in children but can occur in adults too.
How it spreads
Skin-to-skin contact, shared towels, sports equipment, and sometimes through shaving or scratching (it can “seed” to nearby skin).
3. Fungal Infections (Tinea)
What are they?
Fungal infections (often called tinea) can affect skin, feet, groin, scalp, or nails.
Common examples
Ringworm (tinea corporis): circular, scaly rash with a more active border
Athlete’s foot (tinea pedis): itchy scaling between toes or on soles
Jock itch (tinea cruris): itchy groin rash
Scalp fungus (tinea capitis): scaling + broken hairs (more common in kids)
Nail fungus: thickened/discolored nails (requires a specific workup and plan)
How We Diagnose These Conditions
Diagnosis is often made with:
A focused skin exam (sometimes with magnification/dermoscopy)
If needed:
A quick skin scraping test for fungus
Culture or other testing in select cases
Sometimes we evaluate for look-alike conditions (eczema, psoriasis, dermatitis)
Treatment Options
Your treatment depends on which condition you have, the location, and how many spots are present.
1. Treatment: Warts
Common options may include:
In-office freezing (cryotherapy)
Topical treatments (office-prescribed or guided OTC options)
Targeted treatments for stubborn warts (varies by site and age)
2. Treatment: Molluscum
Options depend on age, location, and number of lesions:
Watchful waiting in some cases (it can resolve over time)
In-office treatments to speed clearance (when appropriate)
Guidance to reduce spreading (very important)
3. Treatment: Fungal infections
Topical antifungal medication for many skin/foot/groin infections
Oral antifungal medication in select cases (for scalp infection, extensive disease, or certain nail infections)
Hygiene and prevention steps to reduce recurrence
Pre-Op Instructions (Before Your Visit / Treatment)
(Not surgery—these are “before treatment” tips.)
Before your appointment
Don’t cover the area with heavy makeup or thick ointments right before the visit.
Bring a list of what you’ve tried (creams, sprays, home remedies).
If you suspect a fungal infection:
Avoid applying antifungal cream for 24 hours before your visit if possible (helps us evaluate and test).
Wear clothing that makes the area easy to examine (hands/feet/groin/scalp).
If an in-office procedure is planned (like freezing)
Tell us if you:
Take blood thinners or bruise easily
Have circulation problems in hands/feet or nerve issues
Have a history of strong reactions to prior freezing treatments
Post-Op Instructions (After Treatment)
After wart or molluscum freezing (cryotherapy)
What’s normal
Redness, swelling, tenderness
A blister may form and then crust
Healing often takes 1–2+ weeks depending on location
Care
Keep it clean; gentle soap and water is fine
Do not pick at blisters or scabs
Cover with a bandage if it rubs on clothing/shoes
Call us if you have increasing warmth, pus, fever, or worsening pain
After topical treatments (warts/molluscum/fungus)
Use exactly as directed (consistency matters)
Avoid harsh scrubbing
Wash hands after applying medication unless treating hands
Preventing spread and recurrence (key!)
Don’t share towels, razors, socks, shoes, or nail clippers
Keep feet dry; change socks daily
Wear shower shoes in gyms/pools
Avoid scratching; keep nails short
For molluscum: avoid shaving over bumps and cover lesions for sports when possible
Frequently Asked Questions
Are Warts, Molluscum, & Fungal contagious?
Yes—all three can spread through contact or shared surfaces. The good news: treatment plus prevention steps can greatly reduce spread.
How can I tell which one I have?
They can look similar. In general:
Warts: rough/raised, can have tiny black dots, common on hands/feet
Molluscum: smooth, dome-shaped bumps with a small central dimple
Fungus: scaly, itchy rash (often ring-shaped on body or between toes)
A quick exam is often the fastest way to confirm.
Do warts go away on their own?
Some do, but it can take months to years. Treatment often speeds improvement—especially for painful plantar warts or spreading warts.
Why do my child’s molluscum bumps keep spreading?
Scratching, rubbing, and shaving can spread it to nearby skin. We’ll show you how to reduce “autoinoculation” and discuss treatment options.
Is ringworm caused by a worm?
No. “Ringworm” is a nickname for a fungal infection that often forms a ring-like rash.
When should I worry about a fungal infection?
See a dermatologist promptly if:
It’s on the scalp (especially in children)
It’s widespread, painful, oozing, or not improving
You have diabetes, immune suppression, or frequent recurrences
Can I use OTC products first?
Often yes. Many mild fungal infections and some warts can start with OTC care—but if it’s persistent, spreading, painful, or unclear, a medical evaluation saves time and frustration.
When should I call the office after treatment?
Call if you have:
Severe blistering, increasing pain, spreading redness
Drainage/pus, fever
A rash that rapidly worsens or spreads despite treatment
