 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
B. Skin Cancer Types
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
A. Skin Cancer Diagnosis
B. Skin Cancer Types
- Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
- Melanoma
- Merkel Cell Carcinoma
Cutaneous T-Cell Lymphoma (CTCL)
- Primary Cutaneous B-Cell Lymphoma (PCBCL)
- Metastatic Cancers
- Sarcoma
C. Skin Cancer Treatment
- Mohs Micrographic Surgery
- Surgical Excision
- Electrodessication & Curettage(ED&C)
- Radiation Referral Coordination
D. Pre-Cancerous Lesions
- Actinic Keratosis (AK)
- Atypical(Dysplastic) Nevi
- Field Cancerization Treatment
- Photodynamic Therapy (PDT)
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Cutaneous T-Cell Lymphoma (CTCL)
(A rare lymphoma that can start in the skin and sometimes look like eczema or psoriasis)
1. What Is CTCL?
Cutaneous T-Cell Lymphoma (CTCL) is a rare type of non-Hodgkin lymphoma where certain immune cells (T-cells) become abnormal and collect in the skin. CTCL can sometimes involve the blood, lymph nodes, or other organs.
The most common CTCL types are:
Mycosis fungoides (MF) (often slow-growing)
Sézary syndrome (SS) (a less common form that involves skin and blood)
Important: Many people live for years with CTCL that is treatable and manageable—especially in early stages.
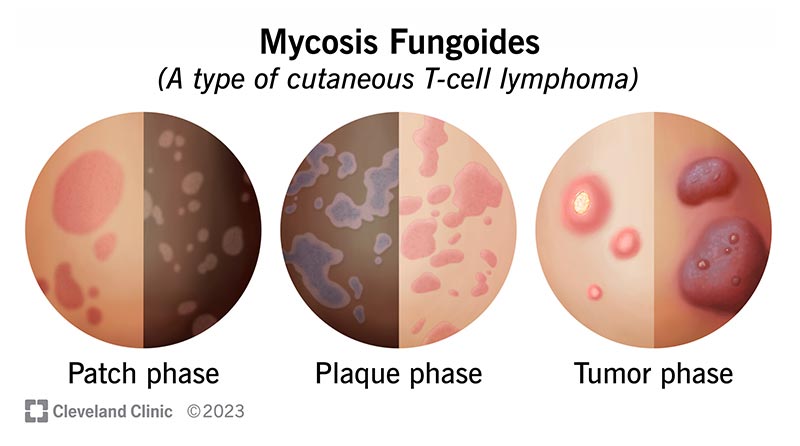
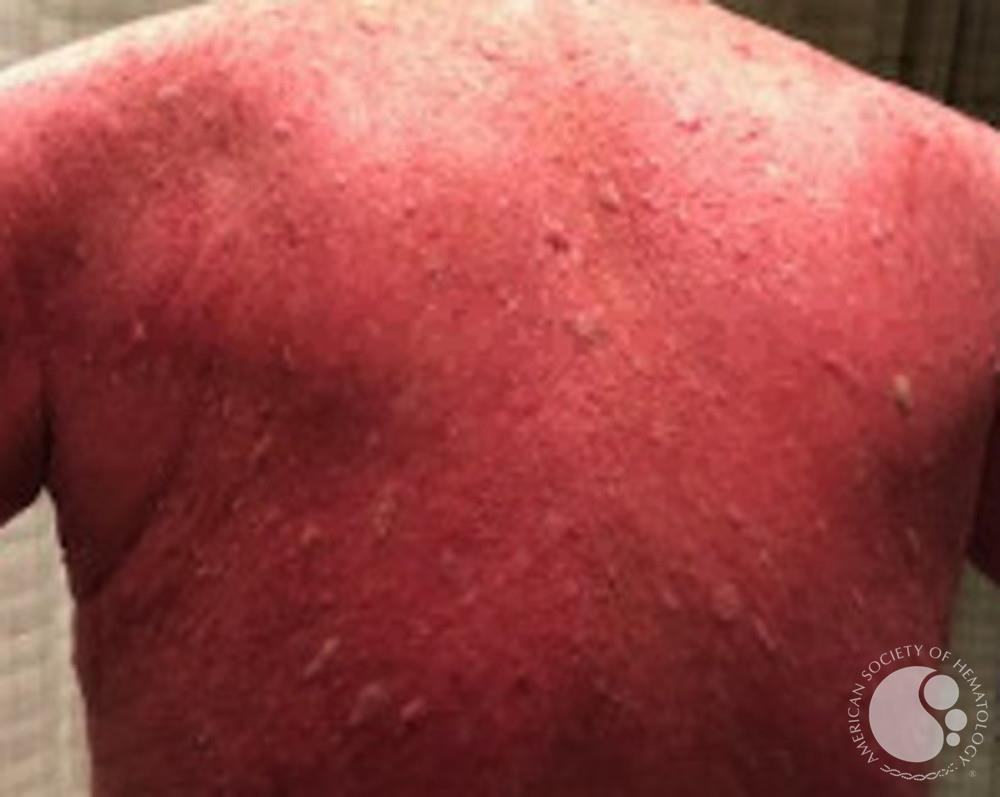
2. What Does CTCL Look Like?
CTCL can vary, but common skin findings include:
Dry, scaly patches that may resemble eczema
Thicker plaques (raised, more firm areas)
Itching, sometimes severe
In more advanced disease: tumors, widespread redness (erythroderma), or enlarged lymph nodes
CTCL often appears on trunk, buttocks, hips, or areas covered by clothing, and it may come and go or respond only partially to typical rash treatments.
3. Why CTCL Can Be Hard to Diagnose
Early CTCL can mimic benign rashes, and diagnosis often requires:
More than one biopsy
Clinic-pathology correlation (matching what we see on your skin with what the pathologist sees under the microscope)
4. How CTCL Is Diagnosed
Evaluation may include:
Full skin exam (sometimes measuring body surface area involved)
Skin biopsy (sometimes multiple samples)
Blood tests (especially if Sézary syndrome is suspected)
Lymph node exam and, in selected cases, imaging or specialist referral
5. Treatment Options
Treatment is customized to your stage, symptoms, and goals. Many patients—especially with early MF—are treated with skin-directed therapies.
Common skin-directed treatments
Prescription topical therapies (anti-inflammatory and/or anti-cancer creams, depending on plan)
Phototherapy (light therapy such as narrowband UVB or PUVA in appropriate cases)
Targeted spot treatments (selected lesions)
When systemic treatment is needed
If disease is more extensive or involves blood/lymph nodes, CTCL care may include systemic medications and coordination with oncology/hematology.
6. Pre-Op Instructions
(For biopsy or phototherapy — not surgery)
Before a CTCL evaluation / biopsy
Bring a list of all topicals, prescriptions, OTC products, and supplements
Take photos of the rash during flares (many rashes change day-to-day)
Tell us if you have:
Enlarged lymph nodes, fevers, night sweats, weight loss
Severe itch impacting sleep
If you’re using strong topical steroids, don’t stop abruptly—we’ll guide what to do before biopsy.
If phototherapy is planned
Avoid tanning/sunburn
Tell us about any medications that cause sun sensitivity
Arrive with clean skin (no heavy oils/perfumes on treatment areas)
7. Post-Op Instructions
After a skin biopsy
Keep the bandage on and dry for 24 hours (unless instructed otherwise)
Then daily: clean gently, pat dry, apply ointment if instructed, cover with a clean bandage
Avoid soaking (pools/hot tubs/baths) until healed
Call if you have increasing redness, warmth, swelling, pus, fever, or bleeding that won’t stop with pressure
After starting CTCL treatment
Many therapies require weeks to months to judge response
Keep follow-ups so we can adjust treatment and manage itch
If phototherapy is used, mild redness is common; report painful “sunburn” reactions
Frequently Asked Questions
Is Cutaneous T-Cell Lymphoma (CTCL) contagious
No. CTCL is not contagious.
Is CTCL always aggressive?
Not always. Mycosis fungoides often progresses slowly and can be managed long-term, especially when found early.
Why might I need more than one biopsy?
Early CTCL can resemble eczema or psoriasis, and diagnosis may require multiple biopsies plus correlation with your clinical pattern.
What is Sézary syndrome?
Sézary syndrome is a form of CTCL where abnormal T-cells are found in the blood, and skin redness may be widespread.
Can phototherapy help CTCL?
Yes. Phototherapy (like narrowband UVB or PUVA) is an important skin-directed treatment for many patients with MF.
Will I be referred to oncology?
Sometimes. Many early cases are managed primarily with dermatology skin-directed therapy, but more advanced disease may involve hematology/oncology as part of a team approach.
When should I call urgently?
Seek urgent care for trouble breathing, severe weakness, or rapidly worsening, painful skin with fever. Call our office promptly for rapidly spreading redness, new tumors, painful sores, or swollen lymph nodes.
