 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
D. Pre-Cancerous Lesions
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
A. Skin Cancer Diagnosis
B. Skin Cancer Types
- Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
- Melanoma
- Merkel Cell Carcinoma
- Cutaneous T-Cell Lymphoma (CTCL)
- Primary Cutaneous B-Cell Lymphoma (PCBCL)
- Metastatic Cancers
- Sarcoma
C. Skin Cancer Treatment
- Mohs Micrographic Surgery
- Surgical Excision
- Electrodessication & Curettage(ED&C)
- Radiation Referral Coordination
D. Pre-Cancerous Lesions
Actinic Keratosis (AK)
- Atypical(Dysplastic) Nevi
- Field Cancerization Treatment
- Photodynamic Therapy (PDT)
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Actinic Keratosis (AK)
1. What is an Actinic Keratosis?
An actinic keratosis (AK) is a precancerous growth caused by long-term UV exposure from the sun or indoor tanning. AKs commonly feel like rough, scaly patches and often appear on sun-exposed areas such as the face, scalp, ears, forearms, and backs of the hands.
AKs are treated because some can progress to squamous cell carcinoma (SCC) over time.
2. What do AKs look and feel like?
AKs can appear as:
Rough, sandpaper-like spots (sometimes easier to feel than see)
Red, pink, tan, or skin-colored patches
Scaly or crusted areas
Occasionally tender, itchy, or burning
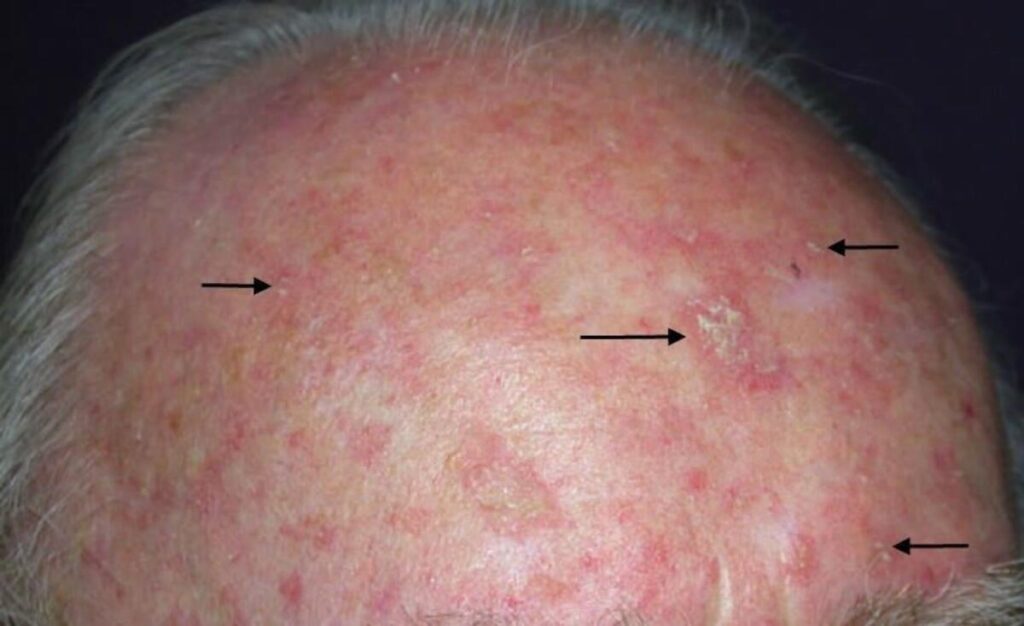
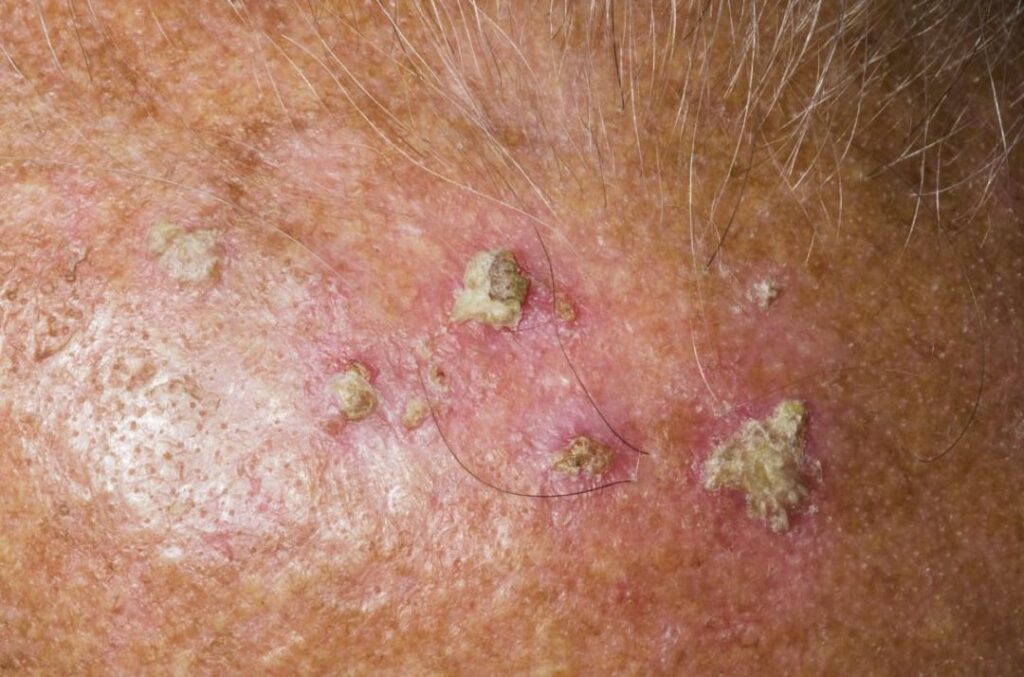
3. Why AKs matter
Having AKs means your skin has had significant UV damage, and you may be at increased risk for skin cancer, which is why ongoing skin exams are important.
4. How AKs are diagnosed
AKs are often diagnosed with a skin exam (sometimes using dermoscopy). If a spot looks thicker, rapidly changing, painful, ulcerated, or “different,” your dermatologist may recommend a biopsy to rule out skin cancer.
5. Treatment Options
Your dermatologist will recommend treatment based on the number of AKs, location, and how thick they are.
Spot Treatments
Cryotherapy (Freezing)
Liquid nitrogen freezes the AK so the damaged cells slough off as the skin heals. It’s one of the most common in-office treatments.
Curettage or Shave Removal (Selected cases)
Used for thicker AKs or when SCC needs to be ruled out (often followed by pathology).
Field Treatments (for “sun-damaged areas” with multiple AKs)
If you have many AKs in one region (like the scalp, forehead, or forearms), your dermatologist may recommend a “field” approach—treating the broader area where AKs form.
Common options include:
Prescription topical therapies
Photodynamic therapy (PDT) (medicine applied, then activated by a specific light)
(Your dermatologist will recommend what fits your skin, schedule, and risk.)
6. Pre-Op Instructions (Before AK Treatment)
Before Cryotherapy (Freezing)
No fasting is needed.
Tell us if you:
Take blood thinners or bruise easily
Have allergies to adhesives or topical products
Avoid applying lotion/makeup directly over the area the day of treatment.
Before Topical “Field Therapy” (if prescribed)
Let us know if you have a history of severe reactions to topical medications.
Plan for temporary redness/irritation (timing varies by medication and treatment plan).
Before Photodynamic therapy (if scheduled)
Arrive with clean skin (no makeup, sunscreen, or heavy moisturizers on the treatment area).
Plan your day so you can avoid bright light/sun exposure afterward as instructed by your office.
7. Post-Op Instructions (After AK Treatment)
After Cryotherapy
Normal expectations:
Redness, swelling, stinging for a short time
A blister may form, then crust and heal
Care:
Keep it clean; gentle soap and water is fine.
Don’t pick at scabs.
Call the office if you have increasing redness, warmth, pus, or worsening pain.
After Topical Field Therapy
Normal expectations:
Redness, dryness, peeling, crusting (this can mean the medication is working)
Care tips:
Use only products your dermatologist recommends on the treated area.
Avoid harsh exfoliants, retinoids, or acids unless approved.
Strict sun protection is essential.
After Photodynamic therapy
Normal expectations:
Redness and sensitivity (similar to a sunburn), sometimes swelling and peeling
Critical instruction:
Avoid bright light/sun exposure for the exact timeframe your office provides.
8. Prevention & Long-Term Care
Daily broad-spectrum sunscreen
Hats / sun-protective clothing
Avoid tanning beds
Regular skin exams to monitor for new AKs or skin cancer
Frequently Asked Questions
Are Actinic Keratoses (AKs) skin cancer?
AKs are precancerous—not skin cancer—but some can develop into squamous cell carcinoma, which is why treatment and monitoring are recommended.
Why do I keep getting AKs?
AKs are a sign of cumulative UV damage. Even after treatment, new AKs can develop over time, especially on chronically sun-exposed areas.
Does cryotherapy hurt?
Most patients feel a brief stinging or burning sensation. Tenderness afterward is usually mild and temporary.
Will treatment leave a scar?
Most AK treatments heal well. Some people may notice temporary color change or a small mark, especially after freezing. Your dermatologist will recommend an approach that balances effectiveness and cosmetic outcome.
How long does it take to heal?
Healing depends on the treatment and the body area. Many cryotherapy spots heal over 1–3 weeks; field treatments and PDT may involve a longer visible recovery period.
When should I call the office?
Call if you notice:
Rapid growth, increasing pain, ulceration, or bleeding
A spot that doesn’t heal
Signs of infection (spreading redness, warmth, pus, fever)
