 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
B. Skin Cancer Types
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
A. Skin Cancer Diagnosis
B. Skin Cancer Types
Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
- Melanoma
- Merkel Cell Carcinoma
- Cutaneous T-Cell Lymphoma (CTCL)
- Primary Cutaneous B-Cell Lymphoma (PCBCL)
- Metastatic Cancers
- Sarcoma
C. Skin Cancer Treatment
- Mohs Micrographic Surgery
- Surgical Excision
- Electrodessication & Curettage(ED&C)
- Radiation Referral Coordination
D. Pre-Cancerous Lesions
- Actinic Keratosis (AK)
- Atypical(Dysplastic) Nevi
- Field Cancerization Treatment
- Photodynamic Therapy (PDT)
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Basal Cell Carcinoma (BCC)
1. What is Basal Cell Carcinoma?
Basal Cell Carcinoma (BCC) is the most common type of skin cancer. It usually grows slowly and rarely spreads to distant parts of the body—but it can grow deeper and damage nearby skin and tissue if not treated.
The good news: when found early and treated properly, BCC is highly treatable.
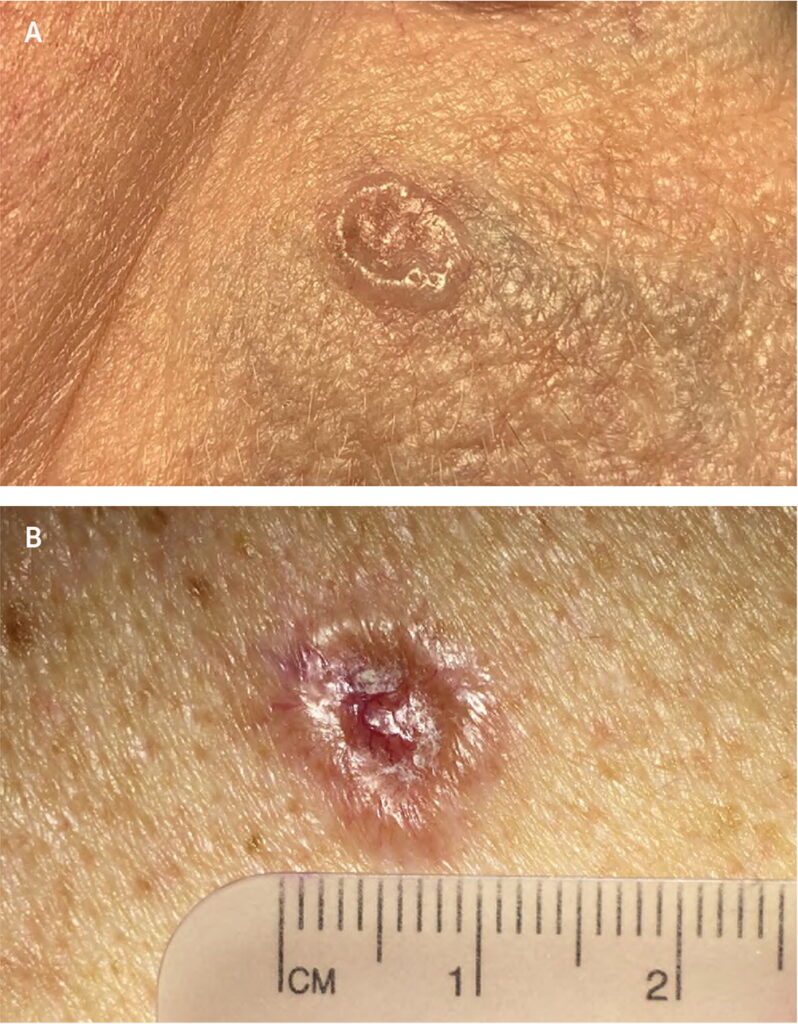
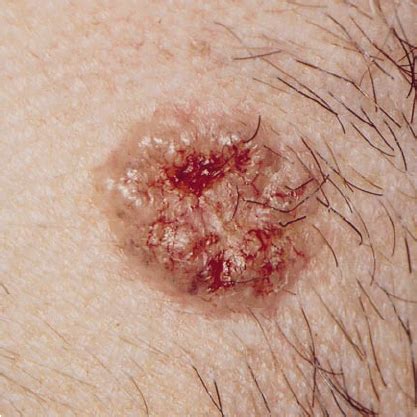
2. What does BCC look like?
BCC can look different from person to person. Common appearances include:
A shiny or pearly bump (sometimes pink or skin-colored)
A sore that doesn’t heal or heals and comes back
A pink patch or growth with a slightly raised border
A scar-like, flat, firm area
A spot with visible small blood vessels
BCC is often found on sun-exposed areas like the face, scalp, ears, neck, and arms, but it can occur anywhere.
3. Why does BCC happen?
Most BCCs are related to cumulative sun exposure and UV damage over time.
Risk factors can include:
A history of frequent sun exposure or sunburns
Tanning bed use
Fair skin (but BCC can occur in all skin types)
Prior skin cancer
Weakened immune system
4. How is BCC diagnosed?
BCC is diagnosed by a dermatologist with:
Skin exam (often with dermoscopy for magnified detail)
Skin biopsy to confirm the diagnosis under the microscope
5. Treatment Options
Treatment depends on the type of BCC, size, location, and your medical history. Common options include:
Surgical treatments
Excision (removes the cancer plus a margin of normal skin)
Mohs Micrographic Surgery (often used for face/scalp/ears, recurrent tumors, or high-risk areas; preserves healthy tissue while maximizing cure)
Curettage & electrodessication (ED&C) (scrape + cautery; used for select low-risk BCCs)
Non-surgical options (select cases)
Topical medications, photodynamic therapy, or radiation may be considered in specific situations.
Your dermatologist will recommend the safest option for complete removal and best cosmetic outcome.
6. Pre-Op Instructions (Before BCC Treatment)
These instructions apply to biopsy, excision, or Mohs—your office may tailor them for you.
1–7 days before (important)
Tell us if you take blood thinners (including aspirin, warfarin, clopidogrel, apixaban, rivaroxaban) or have a bleeding disorder. Do not stop prescribed blood thinners unless your prescribing doctor instructs you.
Tell us if you have:
– Allergies (medications, adhesives, antiseptics)
– A history of poor wound healing or keloids
-A pacemaker/defibrillator (rarely relevant, but good to know)
Day of procedure
Eat normally (no fasting unless we specifically tell you)
Take usual medications unless instructed otherwise
Wear comfortable clothing and avoid makeup/lotions over the site (especially for facial procedures)
Bring a list of medications and supplements
7. Post-Op Instructions (After BCC Treatment)
After biopsy (if done)
Keep bandage on and dry for ~24 hours (unless instructed otherwise)
Then: gentle wash → pat dry → thin layer of ointment → fresh bandage daily
Avoid soaking (pools/hot tubs) until healed or stitches removed
After excision or Mohs surgery
Expect some swelling, bruising, or tightness—especially on the face
Limit strenuous activity and heavy lifting for the time recommended (often several days)
Keep the area clean and covered as instructed
Protect the area from sun (sun can darken scars)
Bleeding
If bleeding occurs:
Apply firm pressure for 15 minutes without checking
If still bleeding, repeat once
If bleeding continues after 30 minutes, contact the office
8. Call us urgently if you notice
Increasing redness, warmth, swelling, pus, fever
Worsening pain after the first day
Bleeding that won’t stop with pressure
9. Follow-up and Prevention
Even after successful treatment, patients who have had BCC are at higher risk for developing another skin cancer, so ongoing skin exams and sun protection matter.
Frequently Asked Questions
Is basal cell carcinoma life-threatening?
BCC rarely spreads, but it can cause significant local damage if left untreated. Early treatment is strongly recommended.
How do you confirm BCC?
A skin biopsy confirms the diagnosis by examining the tissue under a microscope.
What’s the best treatment for BCC?
There isn’t one “best” treatment for everyone. Options depend on the tumor’s location, size, subtype, and risk level. Surgery is common, and Mohs is often chosen for higher-risk sites like the face because it can preserve more healthy tissue.
Will I have a scar?
Any procedure can leave a scar, but careful closure and good wound care can improve healing. Your dermatologist will choose a treatment that balances complete removal and cosmetic outcome.
How long does Mohs surgery take?
Mohs is done in stages. Many patients are in the office for several hours, depending on how many stages are needed.
Can BCC come back after treatment?
It can. That’s why follow-up and regular skin exams are important—especially for patients with prior skin cancer.
What can I do to prevent future skin cancers?
Daily broad-spectrum sunscreen, sun-protective clothing, avoiding tanning beds, and routine dermatologist exams all reduce risk and improve early detection.
