 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
C. Skin Cancer Treatment
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
A. Skin Cancer Diagnosis
B. Skin Cancer Types
- Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
- Melanoma
- Merkel Cell Carcinoma
- Cutaneous T-Cell Lymphoma (CTCL)
- Primary Cutaneous B-Cell Lymphoma (PCBCL)
- Metastatic Cancers
- Sarcoma
C. Skin Cancer Treatment
- Mohs Micrographic Surgery
Surgical Excision
- Electrodessication & Curettage(ED&C)
- Radiation Referral Coordination
D. Pre-Cancerous Lesions
- Actinic Keratosis (AK)
- Atypical(Dysplastic) Nevi
- Field Cancerization Treatment
- Photodynamic Therapy (PDT)
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Surgical Excision (Skin Lesion Removal)
1. What Is Surgical Excision?
A surgical excision is a common in-office procedure where a dermatologist removes a skin lesion (such as a skin cancer, atypical mole, cyst, or other growth) along with a small margin of normal-appearing skin when needed. The area is then typically closed with stitches (sutures).
Excision is used to:
Treat skin cancers (such as BCC, SCC, and some melanomas)
Remove atypical/dysplastic moles
Remove certain benign growths (cysts, lipomas, irritated lesions)
Obtain a complete specimen for diagnosis and to confirm clear margins (when indicated)
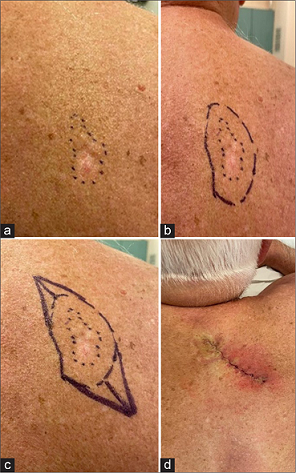
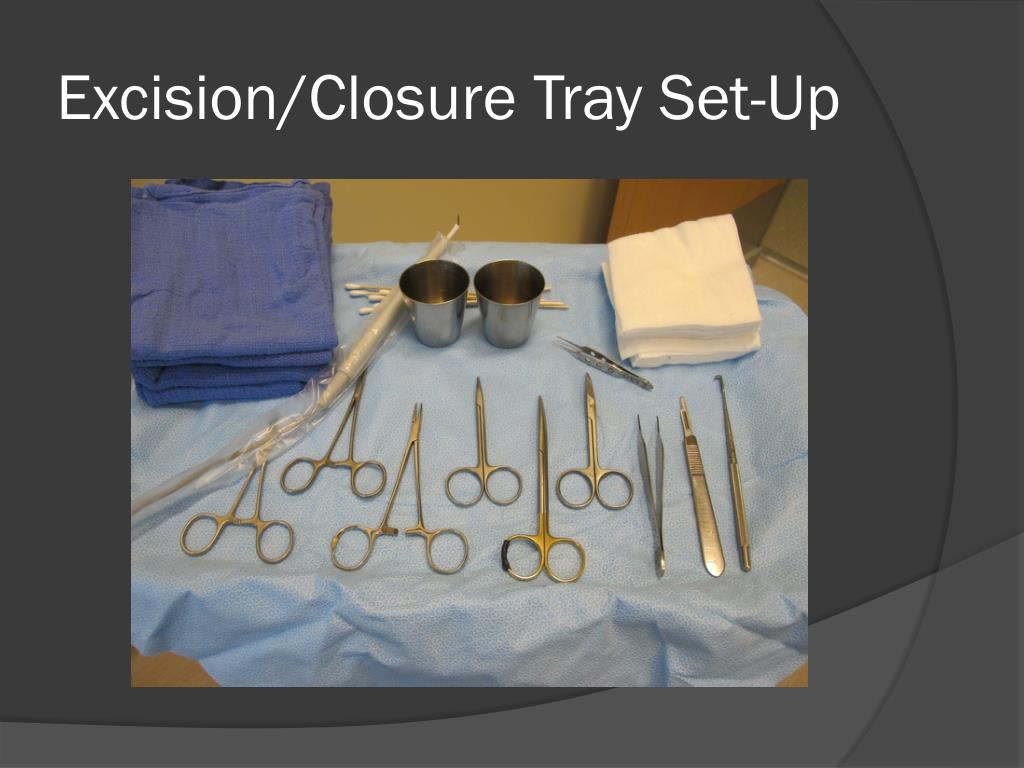
2. What to Expect During Excision
Most excisions are performed in the office with local anesthesia:
Marking & measuring the lesion
Numbing injection (brief sting/burn)
Removal of the lesion (you should not feel pain, only pressure)
Bleeding control
Stitches placed to close the wound
Bandage applied + aftercare instructions
3. Pre-Op Instructions (Before Surgical Excision)
Tell us before your procedure if you:
Take blood thinners (aspirin, warfarin, clopidogrel, apixaban, rivaroxaban, etc.).
- Any blood thinner prescribed by your providers, patient needs to ask the prescribers to see if it’s OK to stop the med prior to surgery, and for how long.
Have a bleeding disorder or bruise easily
Have allergies to lidocaine, antiseptics, or adhesives
Have a history of keloids or poor wound healing
Have had prior infections after procedures

One week before
- Stop drinking alcohol (due to blood thinning effect of alcohol)
- Stop smoking
- stop fish oil supplement
- avoid optional aspirin and NSAIDS: Ibuprofen (Advil®, Motrin®), Naproxen (Aleve®), Aspirin (Bayer®), etc…
The day of your excision
Eat normally (no fasting unless instructed)
Take your regular meds unless told otherwise
Wear comfortable clothing that allows easy access to the area
Avoid lotion/makeup directly over the site
If the excision is on the face/scalp: arrive with a clean face/scalp (no heavy makeup/hair products
4. Post-Op Instructions (After Surgical Excision)
(Your clinician may tailor this to your specific location and closure type.)
First 24 hours
Keep the bandage on and keep the area dry (unless told otherwise)
Mild soreness is common; use pain relief as recommended by your clinician
After 24 hours: daily wound care
Wash hands
Gently clean with mild soap and water
Pat dry
Apply a thin layer of ointment if instructed
Cover with a clean bandage
Continue daily until fully healed or until stitch removal (if applicable).
Activity restrictions
Avoid strenuous exercise, heavy lifting, stretching, or friction on the site as instructed
Avoid swimming/hot tubs/baths (soaking) until cleared—especially with stitches
Bleeding—what to do
Apply firm, steady pressure with clean gauze for 15 minutes without checking
If still bleeding, repeat another 15 minutes
If bleeding continues after 30 minutes of pressure, contact the office
Call the office if you notice
Increasing redness, warmth, swelling, pus, fever
Worsening pain after the first day
Red streaking from the site
The wound opens or stitches come loose
Scar care (after the wound has closed)
Protect the area from sun (sun can darken scars)
Your clinician may recommend silicone gel/sheets or other scar-care options
When Will I Get Results?
If the excised tissue is sent to the lab, results are often available within several business days (timing can vary). We will contact you with:
The diagnosis
Whether margins are clear (if relevant)
Next steps and follow-up
Frequently Asked Questions
Does surgical excision hurt?
Local anesthesia is used. You may feel a brief sting from the numbing injection, but the procedure itself should not be painful. Some soreness afterward is normal.
How long does the procedure take?
Many excisions take 20–45 minutes, depending on location, size, and complexity of closure.
Will I need stitches?
Often yes. Most excisions are closed with stitches. Some areas may use dissolving stitches, while others require removal in the office.
Will I have a scar?
Any excision can leave a scar. Dermatologic closures are designed to optimize healing and appearance. Proper wound care and sun protection help scars fade over time.
When are stitches removed?
Timing depends on location:
Face: often sooner
Body/arms/legs: often later
Your office will provide exact timing based on the site.
Can I exercise after an excision?
Light activity is usually okay, but strenuous exercise and heavy lifting may be restricted—especially if the excision is near a joint or on the back/shoulders/legs where tension can pull on stitches.
What if the pathology report shows skin cancer?
If the excision was performed to treat a known skin cancer, we’ll confirm whether the margins are clear. If margins are not clear or if the tumor is higher risk, additional treatment (including Mohs surgery) may be recommended.
What if I’m on blood thinners?
Many patients can safely have excisions while taking blood thinners, but you must inform your dermatologist. Do not stop prescribed blood thinners without guidance from the prescribing clinician.
How do I know if my wound is infected?
Call us if you develop increasing redness, warmth, swelling, pus, fever, or worsening pain after the first day.
