 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
D. Pre-Cancerous Lesions
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
A. Skin Cancer Diagnosis
B. Skin Cancer Types
- Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
- Melanoma
- Merkel Cell Carcinoma
- Cutaneous T-Cell Lymphoma (CTCL)
- Primary Cutaneous B-Cell Lymphoma (PCBCL)
Metastatic Cancers
- Sarcoma
C. Skin Cancer Treatment
- Mohs Micrographic Surgery
- Surgical Excision
- Electrodessication & Curettage(ED&C)
- Radiation Referral Coordination
D. Pre-Cancerous Lesions
- Actinic Keratosis (AK)
- Atypical(Dysplastic) Nevi
- Field Cancerization Treatment
- Photodynamic Therapy (PDT)
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Metastatic Cancers
(When a cancer from another organ spreads to the skin)
1. What Does “Metastatic Cancer” Mean?
Metastatic cancer means a cancer that started in one part of the body (such as the breast, lung, colon, or kidney) has spread to another location.
When metastatic cancer shows up in the skin, it is called a cutaneous metastasis. These are not primary skin cancers like basal cell carcinoma, squamous cell carcinoma, or melanoma—rather, they represent spread from a cancer elsewhere in the body.
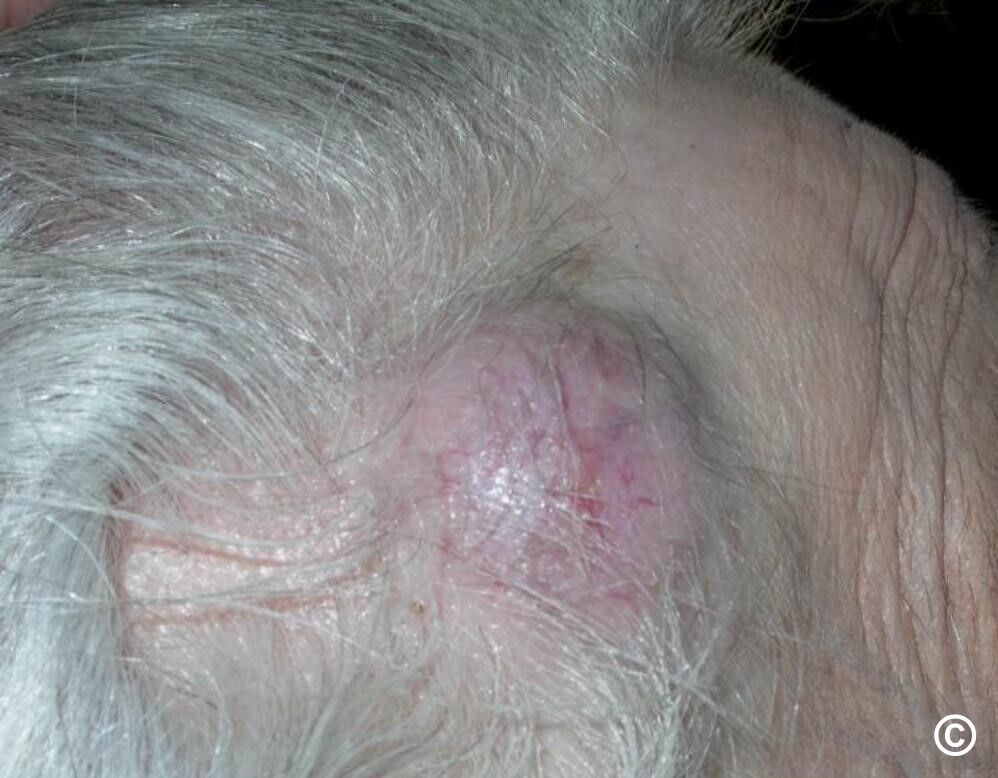
2. What Do Cutaneous Metastases Look Like?
Cutaneous metastases most commonly appear as:
Firm, round or oval bumps (nodules) in or under the skin
Often painless (though they can be tender)
Skin-colored, pink, red, purple—or blue/black in some melanoma metastases
Sometimes multiple lesions appear quickly
Occasionally they can ulcerate (break down) or resemble an infection/rash
They often develop near the original cancer site, but can appear elsewhere.
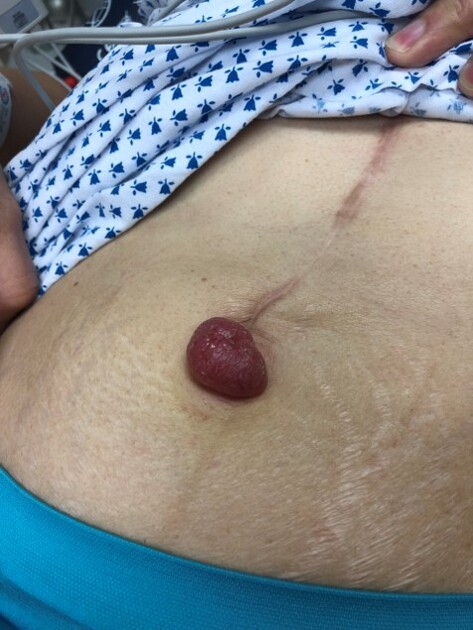
A classic example
A firm nodule at the belly button can be a Sister Mary Joseph nodule, which is an umbilical metastasis from an internal cancer (often gastrointestinal or gynecologic).
3. Which Cancers Most Commonly Spread to Skin?
Cutaneous metastases are uncommon overall, but when they occur, common sources include (patterns differ by sex):
Breast, colon, melanoma, ovarian (more common in females)
Lung, colon, melanoma (more common in males)
Important: Sometimes a skin metastasis can be the first sign of an undiagnosed internal cancer—so a prompt evaluation matters.
4. How We Diagnose Metastatic Cancer in the Skin
Diagnosis typically requires:
a) Skin exam
We evaluate size, firmness, growth rate, and location.
b) Skin biopsy
A biopsy is essential to confirm the diagnosis.
c) Special pathology testing
Pathologists often use immunohistochemistry to help identify where the cancer likely originated.
d) Care coordination
If metastasis is confirmed, we coordinate with your oncology team (or help connect you with one) for further evaluation and treatment planning.
5. How Cutaneous Metastases Are Treated
Treatment is usually focused on the underlying cancer, often with guidance from oncology. Because skin metastases often indicate systemic disease, treatment frequently involves systemic anti-cancer therapy (with additional local treatments in selected cases).
Dermatology may also help with:
Symptom relief (pain, bleeding, irritation)
Wound care if ulceration occurs
Biopsy and diagnosis to guide next steps
6. Pre-Op Instructions
(Not surgery—these are “before your visit/biopsy” tips.)
Before your appointment
Take photos if the lesion changes quickly.
Write down:
When you first noticed it
How fast it’s changing
Any history of cancer (type, treatments, dates)
Bring a list of:
Current medications and supplements
Your oncologist’s contact information (if applicable)
If a biopsy may be done
Tell us if you take blood thinners or bruise easily.
⚠️ Do not stop prescribed blood thinners unless your prescribing clinician instructs you.Tell us about allergies to adhesives, antiseptics, or numbing medicine.
7. Post-Op Instructions
After a skin biopsy
Keep the bandage on and dry for 24 hours (unless instructed otherwise).
After 24 hours, daily:
Gently clean with mild soap and water
Pat dry
Apply a thin layer of ointment if instructed
Cover with a clean bandage
Avoid soaking (pools/hot tubs/baths) until healed.
Call if you develop increasing redness, warmth, swelling, pus, fever, or bleeding that won’t stop with pressure.
After results are available
If results show metastatic cancer, we will:
Review what the biopsy suggests
Coordinate next steps with oncology and/or your treating physicians
Help guide what additional testing may be needed
8. When to Seek Urgent Care
Seek urgent/emergency care if you have:
Rapidly worsening shortness of breath, chest pain, confusion, or severe weakness
Uncontrolled bleeding from a skin lesion
High fever with rapidly worsening skin pain or spreading redness
Call our office promptly if:
A lesion is rapidly enlarging
New lumps appear
A biopsy site shows signs of infection
Frequently Asked Questions
#1
PDT uses a prescription medication plus a specific medical light to activate it. Our office only uses “red light” alone can be used for acne in some settings.
#2
During light exposure, many patients feel stinging, heat, tingling, or burning. We use comfort measures (fans, cooling breaks) as needed.
#3
Most patients have visible redness and irritation for 2–7 days, with peeling that can last up to 10 days, depending on the area and intensity.
#4
Some people can, but many prefer downtime because of redness/peeling. Plan for social downtime of a few days, especially for facial treatments.
#5
PDT can significantly reduce AKs and treat “field” sun damage, but it doesn’t stop future sun damage. Ongoing sun protection and skin checks are key.
#6
PDT is widely used in dermatology. Side effects are usually temporary and localized, most commonly redness, burning, swelling, and peeling.
#7
PDT is commonly used for precancerous lesions (AKs) and some superficial conditions as determined by your dermatologist. Confirmed skin cancers often require other treatments. Your clinician will guide what’s appropriate.
#8
Often yes—especially retinoids and exfoliating acids for several days before and after. We’ll give you an exact list based on your regimen.
#9
Call the office. Light exposure too soon can significantly worsen burning and irritation. Cover up immediately and follow our instructions.
