 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
B. Skin Cancer Types
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
A. Skin Cancer Diagnosis
B. Skin Cancer Types
- Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
- Melanoma
- Merkel Cell Carcinoma
- Cutaneous T-Cell Lymphoma (CTCL)
Primary Cutaneous B-Cell Lymphoma (PCBCL)
- Metastatic Cancers
- Sarcoma
C. Skin Cancer Treatment
- Mohs Micrographic Surgery
- Surgical Excision
- Electrodessication & Curettage(ED&C)
- Radiation Referral Coordination
D. Pre-Cancerous Lesions
- Actinic Keratosis (AK)
- Atypical(Dysplastic) Nevi
- Field Cancerization Treatment
- Photodynamic Therapy (PDT)
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Primary Cutaneous B-Cell Lymphoma (PCBCL)
(A rare lymphoma that starts in the skin)
1. What Is PCBCL?
Primary Cutaneous B-Cell Lymphoma (PCBCL) is a rare type of non-Hodgkin lymphoma made up of B-cells (a type of white blood cell) that begins in the skin.
“Primary cutaneous” means:
It starts in the skin, and
At the time of diagnosis, there is no evidence that it began elsewhere in the body.
Many forms of PCBCL are slow-growing and highly treatable, especially when diagnosed early.
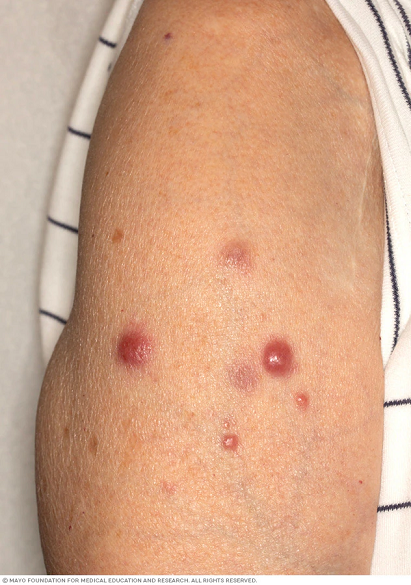
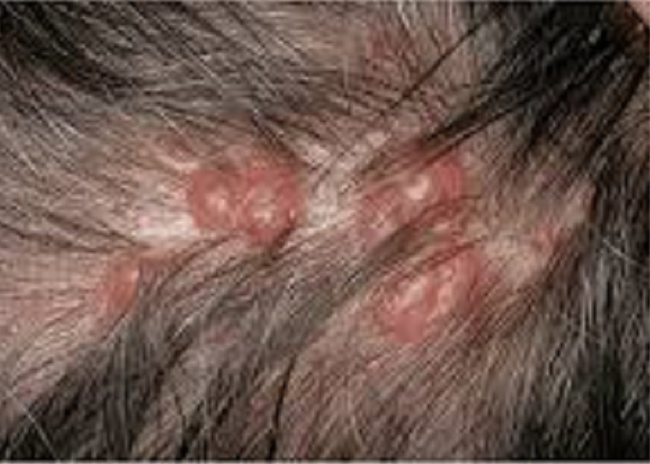
2. What Does PCBCL Look Like?
PCBCL often appears as:
Firm, smooth bumps or nodules
Pink, red, purple, or skin-colored lesions
Usually not scaly
Often not very itchy
May be single or multiple
Common locations:
Scalp / head and neck
Trunk
Sometimes arms or legs (depending on subtype)
Because these bumps can resemble benign growths, evaluation and biopsy are essential.
3. Main Types of PCBCL (Simplified)
Your biopsy helps determine the subtype, which guides treatment and follow-up.
a) Primary Cutaneous Follicle Center Lymphoma
Often on scalp/forehead or upper trunk
Usually slow-growing and very treatable
b) Primary Cutaneous Marginal Zone Lymphoma
Can appear as small bumps or plaques, sometimes multiple
Typically indolent (low-grade) and very treatable
c) Primary Cutaneous Diffuse Large B-Cell Lymphoma (Leg Type)
Less common but more aggressive
Often on the legs
Usually requires more urgent, multidisciplinary treatment
4. How We Diagnose PCBCL
Diagnosis usually includes:
a) Skin Exam
We assess number of lesions, growth pattern, and lymph nodes.
b) Skin Biopsy (Key Step)
A biopsy confirms:
It is a lymphoma
It is B-cell type (special stains are used)
The specific subtype
c) Staging / “Making Sure It’s Primary Cutaneous”
Depending on biopsy results, we may coordinate additional evaluation such as:
Blood tests
Imaging (when indicated)
Referral to hematology/oncology
This helps confirm the lymphoma is skin-limited and guides the safest plan.
5. Treatment Options
Treatment depends on subtype, number of lesions, location, and overall health.
For localized (one or a few) lesions
Common approaches include:
Surgical removal (in selected cases)
Radiation therapy (often very effective for localized disease)
For multiple lesions or recurrent disease
Options may include:
Targeted treatments directed at B-cells
Additional skin-directed or systemic therapy when appropriate
Ongoing monitoring with dermatology ± oncology
Your dermatologist will explain why a particular option fits your situation and what to expect.
6. Pre-Op Instructions
(For biopsy and/or referral-based treatment planning—no special fasting required unless directed by another team.)
Before Your Visit
Take photos of the lesion(s) if they change between visits
Bring a list of:
All medications and supplements
Any prior biopsies, pathology reports, or cancer history
Tell us if you have:
Fevers, night sweats, unexplained weight loss
New enlarged lymph nodes
Rapid growth of a lesion
If a Biopsy Is Planned
Tell us if you:
Take blood thinners or bruise easily
Have allergies to adhesives, antiseptics, or numbing medicine
⚠️ Do not stop prescribed blood thinners unless your prescribing clinician instructs you.
7. Post-Op Instructions
After a Skin Biopsy
Keep the bandage on and dry for 24 hours (unless instructed otherwise)
After 24 hours, daily:
Clean gently with mild soap and water
Pat dry
Apply a thin layer of ointment if instructed
Cover with a clean bandage
Avoid soaking (pools/hot tubs/baths) until healed
Call if you notice increasing redness, warmth, swelling, pus, fever, or bleeding that won’t stop with pressure
After Treatment (General Guidance)
(Your treating team will provide detailed instructions specific to your plan.)
After surgery: follow wound care and activity restrictions provided
After radiation: mild redness, dryness, or irritation can occur—use gentle skin care and sun protection as instructed
Keep follow-up visits so we can monitor for response and recurrence
8. When to Contact Us Promptly
Call our office if you have:
Rapid enlargement of a lesion
New lumps in the neck, armpits, or groin
Persistent fevers, night sweats, or unexplained weight loss
Signs of skin infection at a biopsy or treatment site (worsening pain, pus, spreading redness)
Seek urgent care for severe symptoms such as difficulty breathing or severe weakness.
Frequently Asked Questions
Is PCBCL the same as melanoma or “typical” skin cancer?
No. PCBCL is a lymphoma (cancer of immune cells) that involves the skin. It is different from melanoma, basal cell carcinoma, or squamous cell carcinoma.
Is PCBCL contagious?
No. PCBCL is not contagious.
Is PCBCL serious?
It depends on the subtype. Many PCBCL subtypes are slow-growing and highly treatable, especially when limited to the skin. Some subtypes are more aggressive and need prompt multidisciplinary care.
Why do I need a biopsy?
PCBCL can look like benign bumps or other skin conditions. A biopsy is the only way to confirm the diagnosis and determine the subtype.
Will I need imaging or blood tests?
Sometimes. Additional evaluation helps confirm the lymphoma is primary cutaneous (skin-limited) and guides treatment decisions.
Will I need an oncologist?
Often, yes—especially for staging or certain subtypes. Many patients are cared for by a team that may include dermatology + hematology/oncology.
Can PCBCL come back?
Some types can recur in the skin. That’s why regular follow-up skin exams are important even after successful treatment.
What is the outlook?
Many patients—especially with common indolent subtypes—do very well with appropriate treatment and follow-up. Your team will discuss prognosis based on your specific subtype and staging results.
