 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
B. Skin Cancer Types
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
A. Skin Cancer Diagnosis
B. Skin Cancer Types
- Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
- Melanoma
Merkel Cell Carcinoma
- Cutaneous T-Cell Lymphoma (CTCL)
- Primary Cutaneous B-Cell Lymphoma (PCBCL)
- Metastatic Cancers
- Sarcoma
C. Skin Cancer Treatment
- Mohs Micrographic Surgery
- Surgical Excision
- Electrodessication & Curettage(ED&C)
- Radiation Referral Coordination
D. Pre-Cancerous Lesions
- Actinic Keratosis (AK)
- Atypical(Dysplastic) Nevi
- Field Cancerization Treatment
- Photodynamic Therapy (PDT)
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Merkel Cell Carcinoma
1. What is Merkel Cell Carcinoma?
Merkel cell carcinoma (MCC) is a rare but aggressive type of skin cancer. It often appears as a fast-growing, firm, painless bump on sun-exposed skin (commonly the face, scalp, neck, and arms), but it can occur anywhere.
Because MCC can grow and spread more quickly than many other skin cancers, prompt diagnosis and treatment are very important.
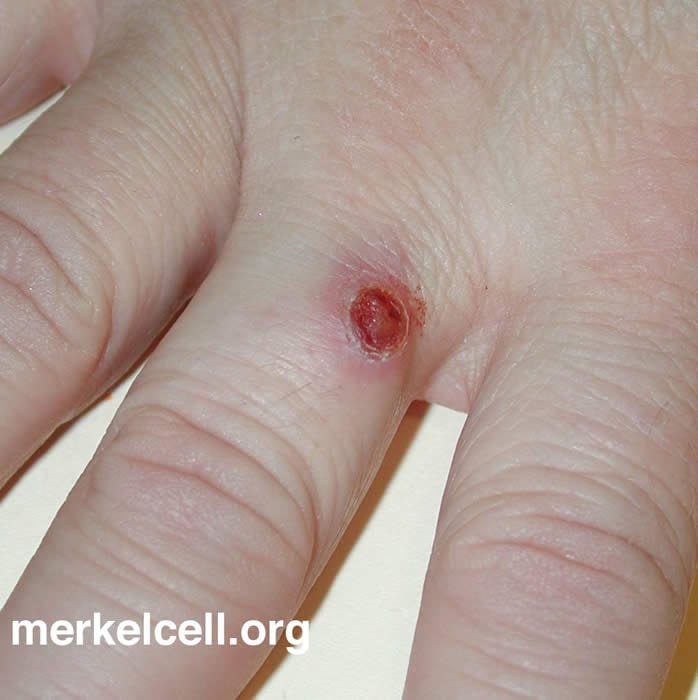
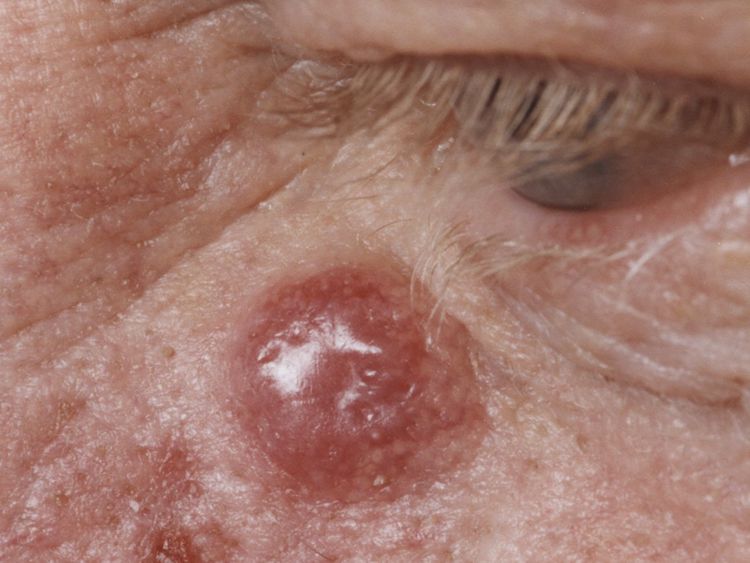
2. What does MCC look like?
MCC often starts as:
A firm, shiny bump or nodule
Pink, red, or purple in color
Usually painless
Grows quickly over weeks to months
Sometimes the surface can break open and bleed
If you have a new spot that is rapidly enlarging or looks “different,” it should be evaluated.
3. Who is at higher risk?
Risk can be higher in people who have:
Significant sun/UV exposure
Older age
A weakened immune system
Evidence of Merkel cell polyomavirus involvement (seen in many cases)
4. How is MCC diagnosed?
Diagnosis typically involves:
Full skin exam and evaluation of the lesion
Skin biopsy (the definitive test)
Pathology review—often with special testing—by an experienced dermatopathologist
Because MCC is rare, specialty pathology experience is important.
5. Treatment overview
Treatment depends on the size/location of the tumor and whether it has spread.
Common treatments may include:
Surgery (Wide Local Excision)
The tumor is removed along with a margin of normal-appearing skin.
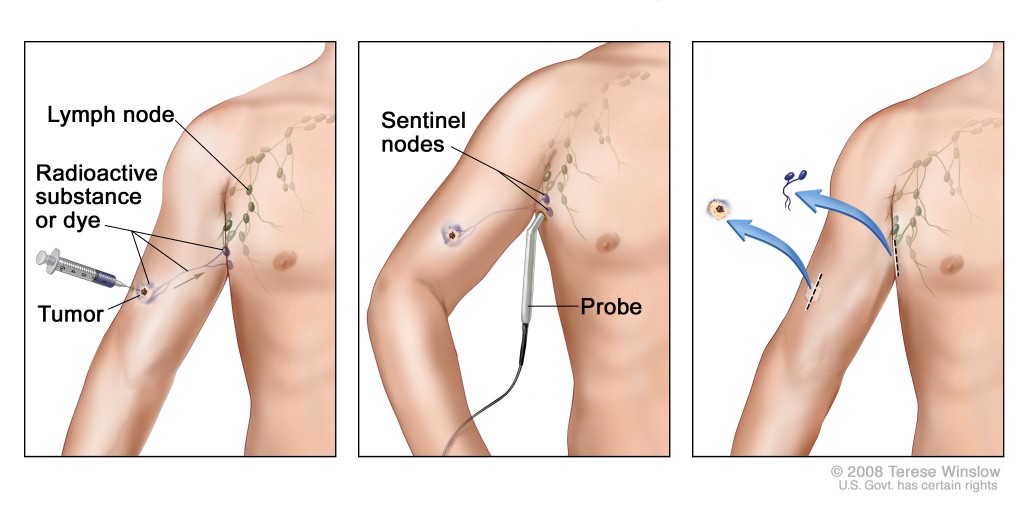
Sentinel Lymph Node Biopsy (SLNB)
Often performed at the time of surgery to check whether cancer cells have spread to nearby lymph nodes.

- SLNB is NOT performed in our dermatology office
- It is done by an oncologic general surgeon
- The procedure is performed in an operating room (OR) setting
It involves lymphatic mapping using specialized imaging (often nuclear medicine guidance)
We coordinate your care and refer you to the appropriate surgical team when SLNB is recommended.
Radiation Therapy
May be recommended after surgery to reduce the chance of recurrence, depending on risk factors.
Advanced disease treatments
For metastatic or advanced MCC, immunotherapy is a common treatment approach.
6. Pre-Op Instructions (Before MCC Treatment)
These are general instructions for biopsy, wide local excision, and/or sentinel lymph node biopsy. Your care team will give you procedure-specific guidance.
6. a) Before your procedure
Tell us if you take blood thinners (including aspirin, warfarin, clopidogrel, apixaban, rivaroxaban) or have a bleeding disorder. Do not stop any prescribed blood thinner unless your prescribing clinician instructs you.
Tell us about:
Medication/adhesive/antiseptic allergies
History of keloids or poor wound healing
Prior anesthesia reactions (if SLNB is planned)
If you’re scheduled for a procedure with anesthesia/sedation, follow fasting instructions exactly.
6. b) Day of procedure
Wear comfortable clothing that allows easy access to the site
Avoid lotion/makeup over the surgical area
Bring a list of medications and supplements
Plan for a driver if sedation is used
7. Post-Op Instructions (After MCC Treatment)
Your team will provide specific instructions. Typical guidance includes:
7. a) Wound care
Keep bandage on and dry for the first 24 hours (unless instructed otherwise).
Then daily:
Gently wash with mild soap and water
Pat dry
Apply a thin layer of ointment if instructed
Cover with a clean bandage
Avoid soaking (baths/hot tubs/pools) until cleared—especially if you have stitches.
7. b) Activity
Avoid strenuous activity/heavy lifting as directed—especially if the wound is on the back, shoulders, arms, legs, or near a joint.
If lymph node biopsy was performed, follow special activity instructions for that area.
7. c) Bleeding
If bleeding occurs:
Apply firm pressure for 15 minutes without checking
Repeat once if needed
If bleeding continues after 30 minutes, contact the office
7. d) Call urgently if you notice
Increasing redness, warmth, swelling, pus, or fever
Worsening pain after the first day
Bleeding that won’t stop with pressure
Red streaking from the wound
7. e) Follow-up after MCC
MCC requires close follow-up because recurrence can occur. Your dermatologist and care team will recommend:
Regular skin exams
Lymph node checks
Imaging or specialist follow-up when appropriate
Frequently Asked Questions
Is Merkel Cell Carcinoma (MCC) the same as melanoma?
No. MCC and melanoma are different skin cancers. MCC is rarer and tends to grow and spread more quickly, which is why timely evaluation and treatment are important.
Does MCC hurt?
Often no—many MCC lesions are painless, which is one reason they can be missed early.
How do you confirm MCC?
A skin biopsy is required. The diagnosis is confirmed by a dermatopathologist examining the tissue under a microscope, often using specialized testing.
Why might lymph nodes be checked?
MCC can spread to nearby lymph nodes. A sentinel lymph node biopsy may be done at the time of surgery to help stage the cancer and guide treatment.
What is the most common treatment?
Treatment often involves wide local excision and may include sentinel lymph node biopsy and radiation therapy, depending on the case.
What should I watch for after treatment?
Notify your care team if you notice:
A new rapidly growing bump
New lumps in the neck, armpit, or groin
New or changing skin lesions
Unexplained swelling near the treated area
Can MCC come back?
Yes. Because MCC can recur, your dermatologist will recommend a structured follow-up plan.
Why can’t SLNB be done in the dermatology office?
SLNB requires specialized imaging, surgical equipment, and an operating room setting. It is performed by an oncologic general surgeon with nuclear medicine support.
Does needing SLNB mean my Merkel Cell Carcinoma has already spread?
No. SLNB is a staging tool. Many patients have negative sentinel nodes, meaning no spread is found.
What happens if the sentinel node is negative?
A negative result is reassuring. Treatment often continues with regular skin exams and follow-up based on Merkel Cell Carcinoma stage.
What happens if the sentinel node is positive?
A positive result means melanoma cells were found in the node. Your care team will discuss:
Additional staging
Possible oncology referral
Tailored surveillance or treatment options
Will I still need follow-up with my dermatologist?
Yes. Regardless of SLNB results, ongoing dermatology follow-up is essential for:
Full-body skin exams
Monitoring for new or recurrent Merkel Cell Carcinoma
Patient education and prevention
