 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
B. Skin Cancer Types
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
A. Skin Cancer Diagnosis
B. Skin Cancer Types
- Basal Cell Carcinoma (BCC)
Squamous Cell Carcinoma (SCC)
- Melanoma
- Merkel Cell Carcinoma
- Cutaneous T-Cell Lymphoma (CTCL)
- Primary Cutaneous B-Cell Lymphoma (PCBCL)
- Metastatic Cancers
- Sarcoma
C. Skin Cancer Treatment
- Mohs Micrographic Surgery
- Surgical Excision
- Electrodessication & Curettage(ED&C)
- Radiation Referral Coordination
D. Pre-Cancerous Lesions
- Actinic Keratosis (AK)
- Atypical(Dysplastic) Nevi
- Field Cancerization Treatment
- Photodynamic Therapy (PDT)
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Squamous Cell Carcinoma (SCC)
1. What Is Squamous Cell Carcinoma?
Squamous Cell Carcinoma (SCC) is a common type of skin cancer that develops from squamous cells in the outer layer of the skin. SCC is often caused by cumulative sun exposure over time.
Most SCCs are highly treatable—especially when found early. However, compared with basal cell carcinoma, SCC has a higher chance of growing deeper and, in some cases, spreading if left untreated. That’s why prompt evaluation and appropriate treatment are important.
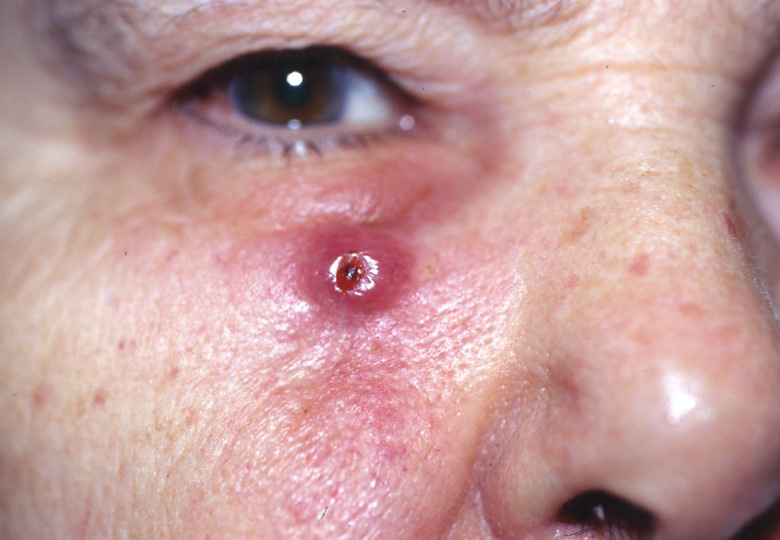
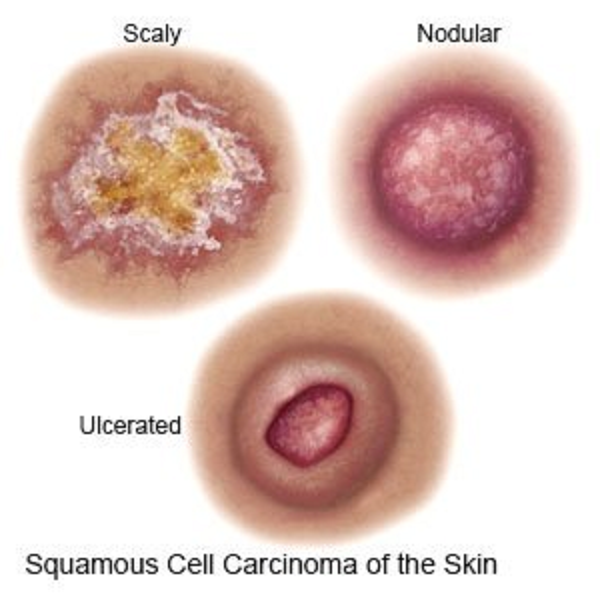
2. What Does SCC Look Like?
SCC can look different from person to person. Common appearances include:
A rough, scaly patch that may crust or bleed
A firm, red bump or nodule
A sore that doesn’t heal (or heals and returns)
A wart-like growth
A growth with a raised edge and a central area that may ulcerate
A tender or painful spot
SCC commonly occurs on sun-exposed areas such as the face, scalp, ears, lips, neck, hands, and forearms—but it can develop anywhere.
3. What Causes SCC?
The most common cause is UV damage from:
Sun exposure over many years
Tanning bed use
Other risk factors include:
- Smoking
- certain subtypes of HPV infections
- A history of actinic keratoses (AKs)
- Previous skin cancer
- Weakened immune system
- Chronic wounds or scars (less common)
Certain occupational or environmental exposures
4. How Is SCC Diagnosed?
Diagnosis typically includes:
Skin examination (often with dermoscopy)
Skin biopsy to confirm the diagnosis under the microscope
A biopsy is the definitive way to determine whether a lesion is SCC and to guide the best treatment plan.
5. Treatment Options for SCC
Treatment depends on the SCC’s size, location, subtype, and risk level. Common options include:
Surgical Treatments
Excision (removal with a margin of normal skin)
Mohs Micrographic Surgery (often preferred for SCC on the face, ears, lips, scalp, hands, recurrent tumors, or higher-risk cases)
Curettage & Electrodessication (ED&C) for select low-risk SCCs in appropriate locations (your dermatologist will determine if suitable)
Other Options (Selected Cases)
In specific situations, your dermatologist may discuss additional options such as topical therapy, radiation therapy, or other targeted approaches, depending on the case.
6. Pre-Op Instructions (Before SCC Treatment)
These instructions apply broadly to procedures like biopsy, excision, ED&C, or Mohs. Your office may tailor instructions based on your treatment plan.
6. a) Before Your Procedure
Tell us if you take blood thinners (including aspirin, warfarin, clopidogrel, apixaban, rivaroxaban) or have a bleeding disorder.
Do not stop prescribed blood thinners unless your prescribing clinician instructs you.Tell us if you have:
Allergies to medications, bandages, or antiseptics
A history of keloids or poor wound healing
A pacemaker/defibrillator (rarely relevant, but helpful to know)
6. b) Day of Procedure
Eat normally unless you were instructed otherwise
Take your usual medications unless instructed otherwise
Wear comfortable clothing and avoid lotions/makeup on the treatment area
Bring a list of medications and supplements
7. Post-Op Instructions (After SCC Treatment)
7. a) If You Had a Biopsy
Keep the bandage on and dry for about 24 hours (unless instructed otherwise)
Then daily: gentle wash → pat dry → thin layer of ointment as directed → fresh bandage
Avoid soaking (baths, pools, hot tubs) until cleared or healed
7. b) If You Had Excision or Mohs Surgery
Mild swelling, bruising, or tightness can be normal—especially on the face
Avoid heavy lifting/strenuous activity for the timeframe your provider recommends
Keep the wound clean, covered, and follow your specific instructions
Protect the area from sun exposure to support optimal scar healing
7. c) Bleeding: What to Do
Apply firm, steady pressure with clean gauze for 15 minutes without checking
If still bleeding, repeat once more for 15 minutes
If bleeding continues after 30 minutes of pressure, contact the office
7. d) Call the Office Urgently If You Notice
Increasing redness, warmth, swelling, pus, or fever
Worsening pain after the first day
Bleeding that won’t stop with pressure
Red streaking from the wound
7. f) Follow-Up & Prevention
After treatment, regular skin exams are important because people who’ve had SCC may be at increased risk for developing additional skin cancers. Your dermatologist will recommend a follow-up schedule and prevention plan, including sun protection.
Call to Action
Early treatment protects your skin and health.
👉 Request an Appointment for SCC Evaluation
Frequently Asked Questions
Is Squamous Cell Carcinoma (SCC) life-threatening?
Most SCCs are highly treatable, especially when caught early. However, SCC can sometimes grow deeper and, in certain cases, spread—so timely treatment is important.
How do you confirm SCC?
SCC is confirmed with a skin biopsy, where a small sample is examined under the microscope.
What’s the difference between Squamous Cell Carcinoma (SCC) and Basal Cell Carcinoma (BCC)?
Both are common skin cancers. In general, SCC has a higher risk of spreading than BCC, which is why evaluation and treatment planning are especially important.
What is Mohs surgery and when is it used for SCC?
Mohs surgery removes the cancer in thin layers while checking the margins under the microscope in real time. It’s commonly used for SCC in high-risk areas (face, ears, lips, scalp, hands), for recurrent tumors, or when tissue preservation is important.
Will I have a scar after treatment?
Any procedure can leave a scar, but careful technique and good wound care help healing. Your dermatologist will choose a treatment that balances complete removal with the best cosmetic outcome.
Can SCC come back after treatment?
It can. That’s why follow-up visits and monitoring are recommended, especially for higher-risk lesions.
What can I do to prevent SCC?
Daily broad-spectrum sunscreen
Sun-protective clothing and hats
Avoid tanning beds
Routine skin exams and self-checks
What should I watch for at home?
Contact your dermatologist if you notice:
A spot that grows, bleeds, crusts, or doesn’t heal
A rough, scaly patch that persists
A tender, painful, or rapidly changing lesion
