 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
B. Skin Cancer Types
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
A. Skin Cancer Diagnosis
B. Skin Cancer Types
- Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
Melanoma
- Merkel Cell Carcinoma
- Cutaneous T-Cell Lymphoma (CTCL)
- Primary Cutaneous B-Cell Lymphoma (PCBCL)
- Metastatic Cancers
- Sarcoma
C. Skin Cancer Treatment
- Mohs Micrographic Surgery
- Surgical Excision
- Electrodessication & Curettage(ED&C)
- Radiation Referral Coordination
D. Pre-Cancerous Lesions
- Actinic Keratosis (AK)
- Atypical(Dysplastic) Nevi
- Field Cancerization Treatment
- Photodynamic Therapy (PDT)
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Melanoma
1. What is melanoma?
Melanoma is a type of skin cancer that starts in pigment-producing cells (melanocytes). It is less common than basal cell carcinoma (BCC) or squamous cell carcinoma (SCC), but it can be more serious because it has a higher chance of spreading if not treated early.
The good news: early detection and treatment are highly effective, which is why skin checks and prompt evaluation of changing moles are so important.
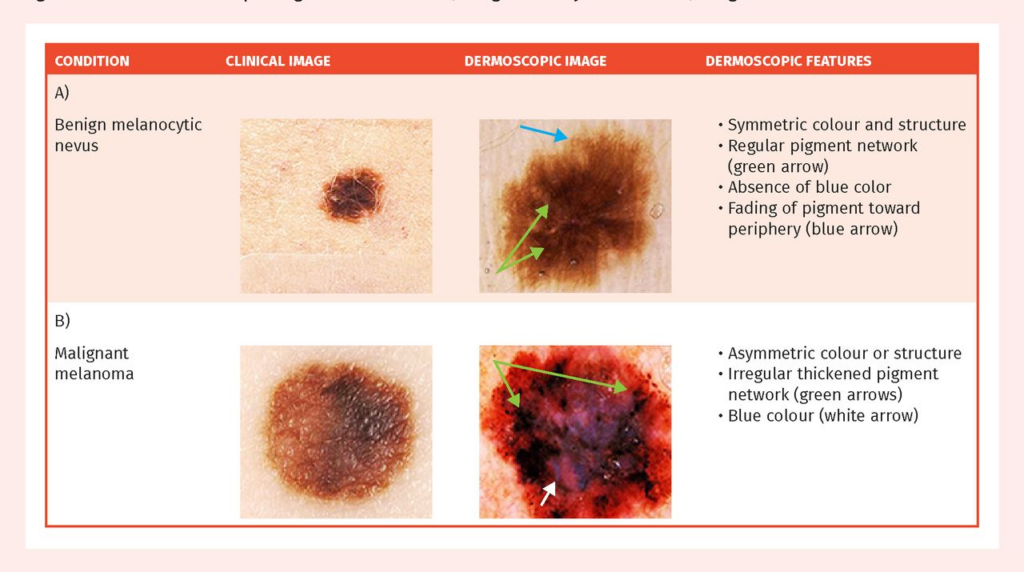
2. What does melanoma look like?
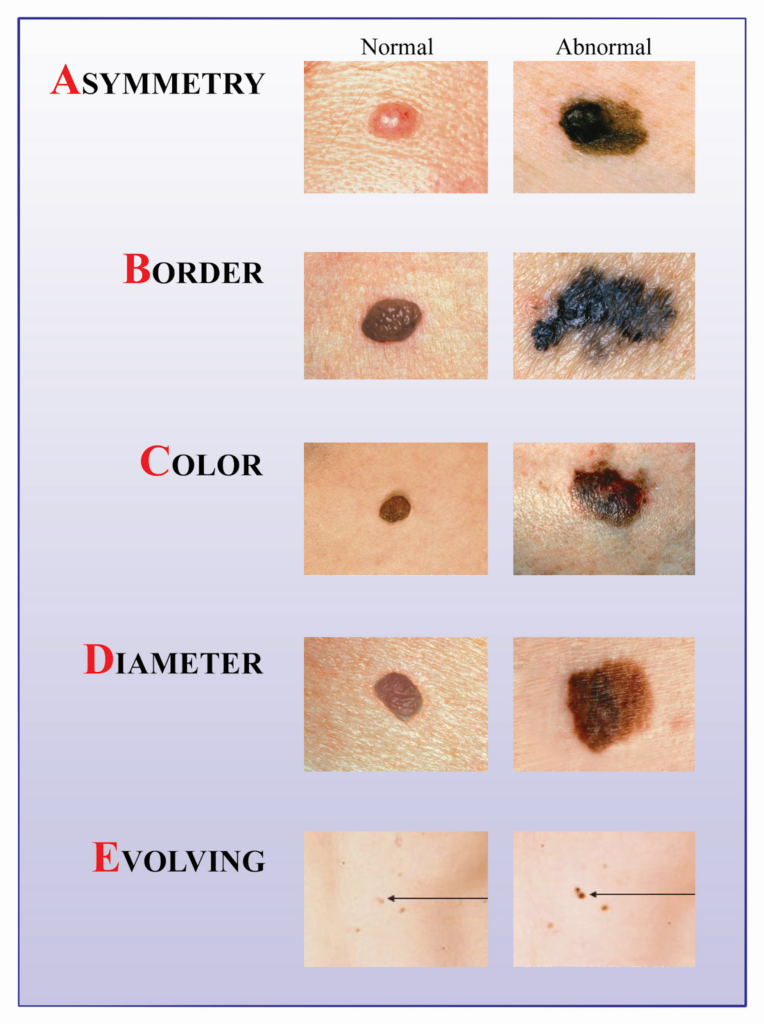
Melanoma can look like a changing mole or a new “different” spot. Dermatologists often teach the ABCDE rule:
A – Asymmetry: one half doesn’t match the other
B – Border: irregular, notched, or blurred edges
C – Color: multiple colors or uneven color (tan, brown, black, red, white, blue)
D – Diameter: often larger than 6 mm (but can be smaller)
E – Evolving: changing in size, shape, color, or symptoms (itching, bleeding)
Another helpful concept is the “ugly duckling” sign: a spot that looks noticeably different from your other moles.
3. Who is at higher risk?
Melanoma can occur in any skin type. Risk is higher if you:
Have a personal or family history of melanoma
Have many moles or atypical/dysplastic nevi
Have a history of intense sun exposure or blistering sunburns
Use (or used) tanning beds
Have a weakened immune system
- Have breast cancer (personal or family history of breast cancer)
- other familial cancer syndromes
4. How is melanoma diagnosed?
Diagnosis typically includes:
Skin exam (often with dermoscopy to see patterns not visible to the naked eye)
Skin biopsy to confirm the diagnosis under the microscope
If melanoma is confirmed, your dermatologist will discuss next steps, which may include additional procedures or referrals depending on depth and risk features.
5. Treatment overview
Treatment depends on the melanoma’s depth and whether it has spread. Many melanomas are treated with:
Wide local excision (surgery to remove the melanoma with a safety margin of normal skin)
In some cases, Sentinel Lymph Node Biopsy(SLNB) may be recommended to check if melanoma has spread to nearby lymph nodes (based on risk factors and pathology)
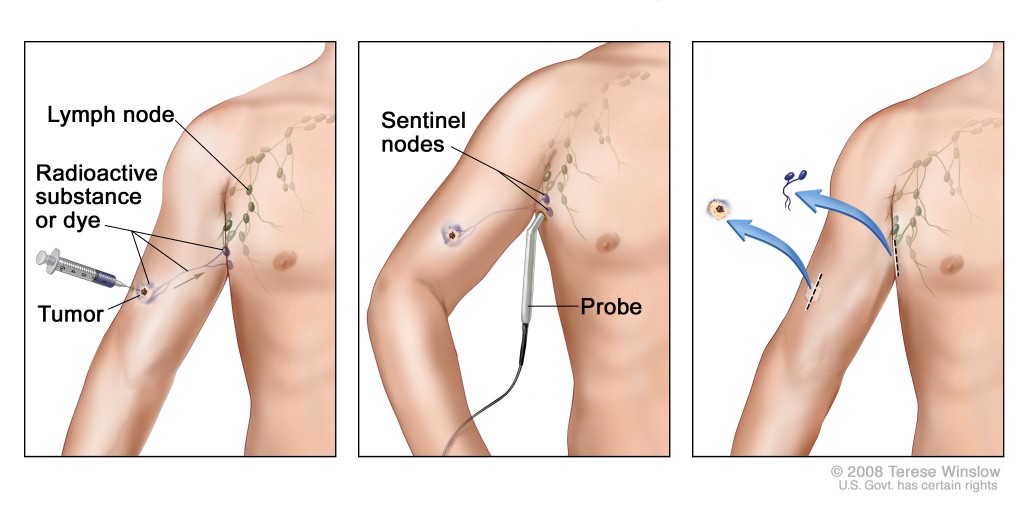

- SLNB is NOT performed in our dermatology office
- It is done by an oncologic general surgeon
- The procedure is performed in an operating room (OR) setting
It involves lymphatic mapping using specialized imaging (often nuclear medicine guidance)
We coordinate your care and refer you to the appropriate surgical team when SLNB is recommended.
If melanoma is more advanced, additional treatments may include systemic therapies (such as immunotherapy or targeted therapy) coordinated with oncology.
6. Pre-Op Instructions
(Before Melanoma Surgery)
These instructions are general and may be adjusted for your specific plan (excision, excision + sentinel node biopsy, etc.).
6. a) 1–7 days before
Tell us if you take blood thinners (including aspirin, warfarin, clopidogrel, apixaban, rivaroxaban) or have a bleeding disorder.
Do not stop prescribed blood thinners unless your prescribing clinician instructs you.
6.a) continued:
Tell us about:
Medication/adhesive/antiseptic allergies
History of keloids or poor wound healing
Prior reactions to local anesthetics
Arrange time off if your procedure site will limit activity.
6. b) Day of procedure
Follow your specific instructions about eating/drinking (especially if sedation or lymph node mapping is planned).
Wear comfortable clothing that allows access to the site.
Avoid lotions, oils, or makeup over the surgical area.
7. Post-Op Instructions (After Melanoma Excision)
Your team will provide specific wound care directions. Typical guidance includes:
7.a) Wound care
Keep the bandage on and dry for the first 24 hours (unless instructed otherwise).
Then daily:
Gently wash with mild soap and water
Pat dry
Apply a thin layer of ointment if instructed
Cover with a clean bandage
Avoid soaking (pools, hot tubs, baths) until cleared—especially if you have stitches.
7. b) Activity
Limit heavy lifting and strenuous exercise as advised (often several days to 2 weeks depending on location and closure).
If the surgery is on the back, shoulders, arms, legs, or near joints, you may need extra activity restrictions to prevent pulling on stitches.
7. c) Bleeding
If bleeding occurs:
Apply firm pressure for 15 minutes without checking
Repeat once if needed
- If bleeding continues after 30 minutes of pressure, contact the office
7. d) Call the office urgently if you notice
Increasing redness, warmth, swelling, pus, fever
Worsening pain after the first day
Bleeding that won’t stop with pressure
Red streaking from the wound
Frequently Asked Questions
Is melanoma curable?
Many melanomas are highly treatable when found early. Treatment success depends on factors such as depth and whether it has spread.
How do you confirm melanoma?
Melanoma is confirmed by a skin biopsy, reviewed under the microscope.
Does melanoma always look black or very dark?
No. Some melanomas can be lighter brown, pink, red, or even skin-colored. Any changing or different-looking lesion should be evaluated.
What is the ABCDE rule?
It’s a guide to warning signs in moles: Asymmetry, Border, Color, Diameter, Evolving.
Will I need lymph node testing?
Not everyone. A sentinel lymph node biopsy is considered in certain cases based on the biopsy report and risk factors. Your dermatologist will explain if it applies to you.
Will I have a scar after melanoma surgery?
Any excision can leave a scar. Careful closure and good wound care help healing, and sun protection helps scars fade more evenly.
Can melanoma come back?
It can. That’s why follow-up skin exams and monitoring are important after treatment.
What should I watch for at home?
Contact us if you notice:
A new or changing mole
A spot that bleeds, crusts, or doesn’t heal
A lesion that looks different from your other moles (“ugly duckling”)
Why can’t Sentinel Lymph Node Biopsy(SLNB) be done in the dermatology office?
SLNB requires specialized imaging, surgical equipment, and an operating room setting. It is performed by an oncologic general surgeon with nuclear medicine support.
Does needing SLNB mean my melanoma has already spread?
No. SLNB is a staging tool. Many patients have negative sentinel nodes, meaning no spread is found.
What happens if the sentinel node is negative?
A negative result is reassuring. Treatment often continues with regular skin exams and follow-up based on melanoma stage.
What happens if the sentinel node is positive?
A positive result means melanoma cells were found in the node. Your care team will discuss:
Additional staging
Possible oncology referral
Tailored surveillance or treatment options
Is SLNB treatment or diagnosis?
SLNB is a diagnostic and staging procedure, not a treatment that removes all melanoma from the body.
Does SLNB leave a scar?
Yes, a small scar is expected. Surgeons aim to minimize scarring while ensuring accurate staging.
