 Pigment & Lesion Disorders
Pigment & Lesion Disorders
A. Acquired Pigment Disorders
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
- Melasma
- Post-Inflammatory Hyperpigmentation (PIH)
Sun Spots (Lentigines)
B. Birthmarks & Congenital Lesions
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Sun Spots (Lentigines)
(“Age spots” or “liver spots” — flat brown spots from sun exposure)
What Are Sun Spots (Lentigines)?
Sun spots, also called solar lentigines (plural: lentigines), are flat brown, tan, or dark spots that develop after years of sun exposure. They commonly appear on areas that get the most sun, such as:
Face
Hands
Shoulders
Chest (“V” of the neck)
Upper back
Sun spots are benign (not cancer), but any new or changing dark spot should be evaluated—because some skin cancers can mimic a “sun spot.”
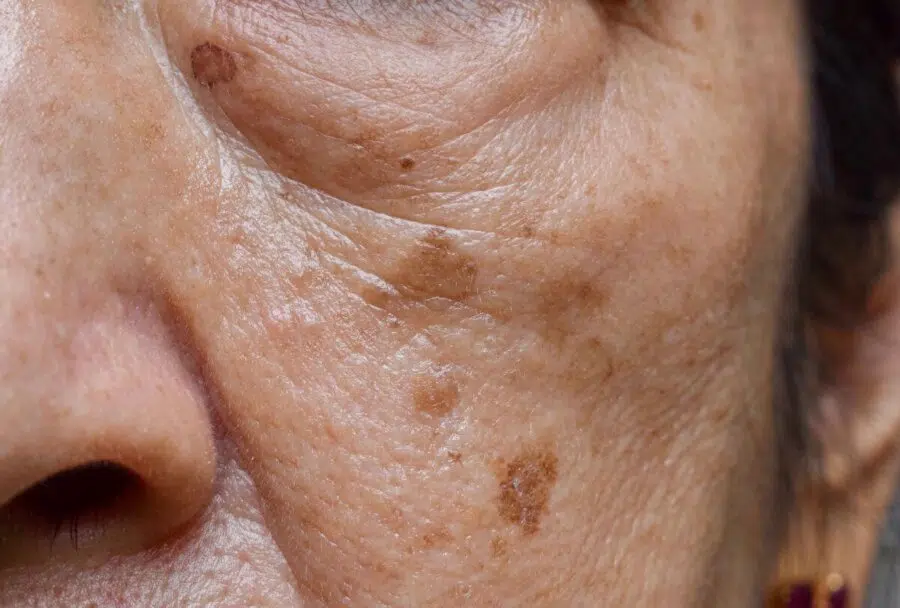
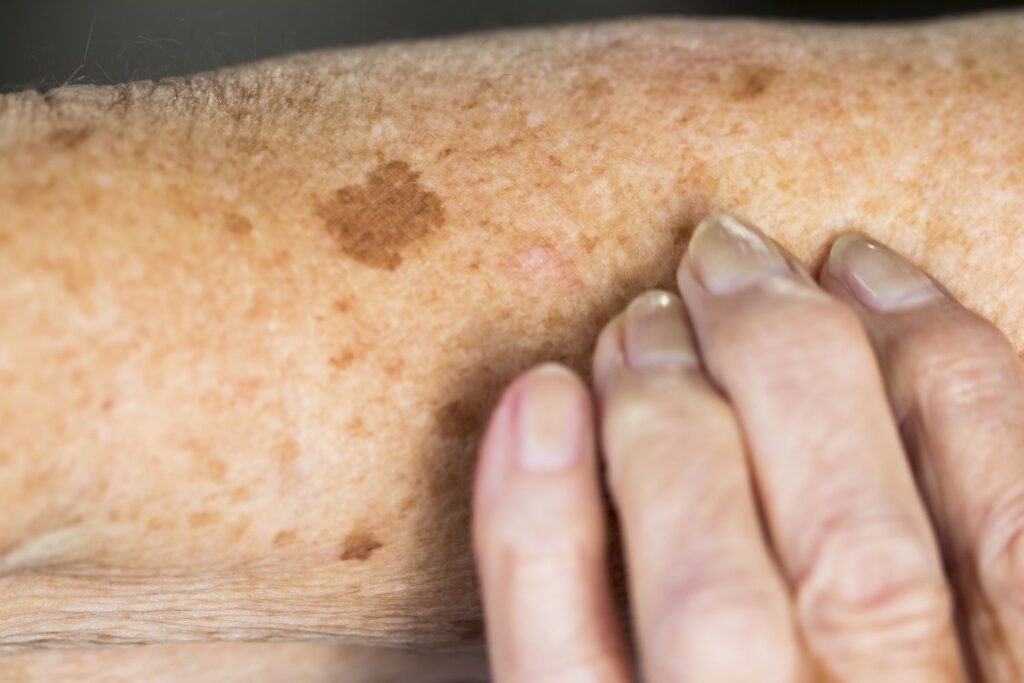
What Do Sun Spots Look Like?
Sun spots are usually:
Flat (not raised)
Tan to dark brown
Well-defined edges
Slow to change over time
They often increase in number with age and sun exposure.
What Causes Lentigines?
Lentigines form when UV exposure stimulates pigment production over time. Common contributors include:
Cumulative sun exposure (including childhood sun)
Tanning (outdoor or indoor)
Genetics and skin type
How We Evaluate Sun Spots
We start with a careful skin exam and may use dermoscopy (a handheld DermLite device) to evaluate pigment patterns.
Important: In our dermoscopy exams:
No photos are taken
No images are stored or uploaded to your chart
(Real-time clinical evaluation only.)
If a spot looks atypical, your dermatologist may recommend a biopsy to confirm the diagnosis.
Treatment Options
Some patients choose to treat lentigines for cosmetic reasons, while others prefer monitoring. Treatment depends on location, skin tone, and your goals.
1. Sun protection (most important)
Daily broad-spectrum sunscreen
Hats and sun-protective clothing
Avoid tanning
This prevents new spots and helps keep treated spots from returning.
2. Topical brightening (gradual improvement)
Medical-grade brighteners and/or prescription options may help lighten spots over time
Best for patients who prefer a gentle, gradual approach.
3. In-office spot treatments (faster results in selected patients)
Depending on your skin type and the spot:
Cryotherapy (freezing) for select lesions
Laser or IPL for widespread sun spots (often considered cosmetic and may not be covered by insurance)
Your dermatologist will advise what’s safest for your skin tone to reduce the risk of irritation or post-inflammatory hyperpigmentation (PIH).
Pre-Op Instructions
(Not surgery—these are “before your treatment” tips.)
Before your evaluation
Avoid tanning or sunburn before your appointment
Make note of any spot that is:
New, changing, bleeding, itchy, or irregular
Bring a list of current skincare products (especially retinoids, acids, brighteners)
Before in-office treatment (freezing / laser / IPL)
Avoid active sun exposure for at least 2 weeks beforehand
Avoid self-tanner in the area
Let us know if you have a history of:
Cold sores (for treatments near the lips)
Dark marks after irritation (PIH)
Keloids or poor wound healing
Stop irritating skincare (scrubs/strong acids/retinoids) as directed
Post-Op Instructions
After cryotherapy (freezing)
What’s normal
Redness, swelling, tenderness
A blister may form, then crust and fall off
Healing usually takes 1–2 weeks (longer on legs)
Care
Gently cleanse daily
Don’t pop blisters or pick scabs
Use a bandage if it rubs on clothing
Call if you develop increasing pain, pus, spreading redness, or fever
After laser / IPL (if performed)
Expect mild redness and “peppering” (darkening of spots) before they flake off
Keep skin moisturized and avoid picking
Strict sunscreen is essential
Avoid hot showers/saunas/excess sweating for 24–48 hours (or as instructed)
After starting topical brighteners
Use exactly as directed (more is not better)
If significant irritation occurs, pause and contact the office—irritation can worsen pigmentation in some patients
When to Contact Us
Schedule evaluation sooner if a “sun spot”:
Is rapidly changing
Has irregular borders or multiple colors
Bleeds, crusts, or won’t heal
Looks very different from your other spots (“ugly duckling”)
Frequently Asked Questions
Are sun spots the same as freckles?
Not exactly. Freckles often darken and lighten with sun exposure. Sun spots (lentigines) tend to be more persistent and related to long-term UV damage.
Are lentigines dangerous?
Lentigines themselves are benign. However, some skin cancers can resemble a sun spot, so any changing lesion should be checked.
Can sun spots go away on their own?
They usually don’t disappear completely without treatment, but they can lighten with consistent sun protection and targeted therapy.
What’s the fastest way to treat sun spots?
In-office treatments (like laser/IPL or select freezing treatments) can provide quicker results than topicals. The best option depends on your skin type and the number of spots.
Will they come back after treatment?
They can—especially with ongoing sun exposure. Daily sunscreen is key to preventing recurrence.
Can treating sun spots cause dark marks (PIH)?
It can in pigment-prone skin, especially if irritation occurs. That’s why we select treatments carefully and emphasize gentle aftercare and sun protection.
Do you need a biopsy for every sun spot?
No. Many are diagnosed clinically (often with dermoscopy). A biopsy is recommended only if a spot looks atypical or uncertain.
