 Pigment & Lesion Disorders
Pigment & Lesion Disorders
B. Birthmarks & Congenital Lesions
• Congenital Nevi (Congenital Melanocytic Nevi, CMN)
(Moles present at birth or that appear in the first weeks of life)
What Is a Congenital Nevus?
A congenital melanocytic nevus (CMN) is a benign mole made of pigment cells that is present at birth or appears within the first few weeks of life.
Congenital nevi vary widely in size, color, thickness, and hair growth. Many remain stable and never cause medical problems.
Types: Size Categories (Why Size Matters)
CMN are commonly described as small, medium, large, or giant based on the lesion’s projected size in adulthood.
In general:
Small/medium CMN: overall melanoma risk is low (often quoted as <1% lifetime), and melanoma is rare before puberty.
Large/giant CMN (and/or multiple CMN): have a higher risk of melanoma and a higher risk of certain neurologic associations.
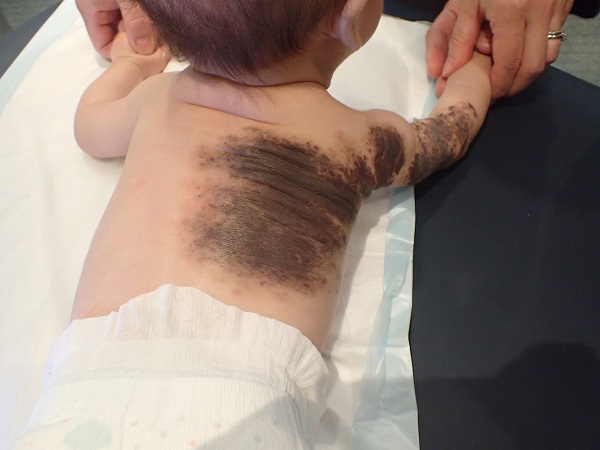

What Do Congenital Nevi Look Like?
Common features include:
Flat or slightly raised brown/tan/black patches
Irregular but stable borders
Sometimes coarse hair
Texture may become more raised or bumpy over time (especially larger lesions)
Some CMN can develop benign “proliferative nodules” (new bumps within the nevus), especially in infancy—these still need evaluation to be safe.
Why We Monitor Congenital Nevi
Most CMN are benign. We monitor because:
A small percentage can develop melanoma, with higher risk in large/giant lesions.
Large/giant CMN can be associated with neurocutaneous melanosis (NCM), a condition involving melanocytic cells in the brain/spinal coverings; published estimates for NCM risk in large/giant CMN are ~10–33%.
How We Evaluate Congenital Nevi
Your visit may include:
Full skin exam and review of personal/family history
Dermoscopy (magnified, lighted evaluation of pigment patterns)
Measurement and documentation of size/location and any “satellite” nevi
Biopsy if a spot has concerning change or an atypical new nodule
For larger lesions or multiple satellites, we may coordinate with pediatrics and other specialists as appropriate.
Treatment Options
Treatment depends on size, location, symptoms, and risk profile:
1. Observation and routine monitoring
Appropriate for many small/medium CMN and stable lesions.
2. Biopsy (if needed)
Recommended if there is a new or changing area that needs clarification.
3. Surgical excision (selected cases)
May be considered for:
Lesions with concerning change
Lesions that are repeatedly irritated/bleeding
Cosmetic or functional reasons
For large/giant CMN, excision is complex and individualized.
Pre-Op Instructions
(Not surgery—these are “before your visit/biopsy/excision” tips.)
Before your CMN appointment
Bring (or upload) older photos if you have them.
Write down:
When you first noticed changes
Any bleeding, pain, or rapid growth
Avoid heavy makeup or self-tanner over the lesion on the day of the visit.
If a biopsy or excision may be done
Tell us if you/your child takes blood thinners or bruises easily.
⚠️ Don’t stop prescribed blood thinners unless the prescribing clinician instructs you.Tell us about adhesive or numbing medicine allergies.
Post-Op Instructions
After a biopsy
Keep bandage on and dry for 24 hours (unless told otherwise).
Then daily: gentle soap + water, pat dry, apply ointment if instructed, cover with a clean bandage.
Avoid soaking (pools/hot tubs/baths) until healed.
Call for increasing redness, warmth, swelling, pus, fever, or bleeding that won’t stop with pressure.
After surgical excision (if performed)
Follow your surgeon’s wound care and activity instructions.
Watch for infection signs and attend scheduled follow-ups.
Long-term monitoring may still be recommended, especially for larger lesions.
When to Contact Us Promptly
Schedule evaluation sooner if a congenital nevus:
Develops a new fast-growing bump within it
Starts bleeding, crusting, or ulcerating without clear injury
Changes rapidly in color, shape, or thickness
Becomes persistently painful
For large/giant CMN, also call if there are new neurologic symptoms (unusual headaches, vomiting, seizures, developmental changes)—these may warrant urgent medical evaluation given NCM associations.
Frequently Asked Questions
Are congenital nevi cancer?
No—CMN are usually benign moles. Some types (especially large/giant) have a higher melanoma risk, which is why follow-up matters.
Should every congenital nevus be removed?
Not always. Many small/medium CMN can be safely monitored. Decisions depend on size, location, changes, and patient preference.
Can a congenital nevus change as a child grows?
Yes. Color, thickness, and hair growth can evolve over time and still be benign. We focus on rapid, asymmetric, or worrisome changes.
What is neurocutaneous melanosis (NCM)?
NCM is a rare condition where melanocytic cells involve the brain/spinal coverings and is more associated with large/giant CMN and multiple satellites; estimates for NCM risk in large/giant CMN are about 10–33%.
What follow-up schedule do you recommend?
It depends on size and risk factors. Many patients benefit from periodic skin checks and home monitoring (photos can help consistency).
What’s the best way to monitor at home?
Take photos every few months in the same lighting and distance.
Watch for the “new bump,” bleeding, or rapid change signs listed above.

 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care Medical Dermatology
Medical Dermatology Non-Cancer Growth
Non-Cancer Growth
 Cosmetic Dermatology
Cosmetic Dermatology