 Pigment & Lesion Disorders
Pigment & Lesion Disorders
A. Acquired Pigment Disorders
 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care
 Medical Dermatology
Medical Dermatology
(Chronic & Inflammatory Skin Diseases)
 Pigment & Lesion Disorders
Pigment & Lesion Disorders
A. Acquired Pigment Disorders
- Melasma
Post-Inflammatory Hyperpigmentation (PIH)
- Sun Spots (Lentigines)
B. Birthmarks & Congenital Lesions
 Non-Cancer Growth
Non-Cancer Growth
 Surgical Dermatology (Non-Cancer Procedures)
Surgical Dermatology (Non-Cancer Procedures)
 Cosmetic Dermatology
Cosmetic Dermatology
• Post-Inflammatory Hyperpigmentation (PIH)
(Dark marks that appear after acne, eczema, irritation, or injury)
1. What Is PIH?
Post-Inflammatory Hyperpigmentation (PIH) is darkening of the skin that happens after inflammation or injury. It’s your skin’s natural response: inflammation can signal pigment-producing cells to make extra melanin, leaving a brown, gray-brown, or even blue-gray mark where the skin was irritated.
PIH is not dangerous and not contagious, but it can take time to fade—especially without the right plan.
2. What Causes PIH?
PIH can follow almost any inflammatory skin event, including:
Acne (especially picked or cystic acne)
Eczema / dermatitis
Insect bites
Rashes or allergic reactions
Cuts, scrapes, burns
Waxing, threading, shaving irritation
Procedures (if the skin becomes inflamed afterward)
PIH is more common and often more noticeable in medium to deeper skin tones, but it can affect anyone.
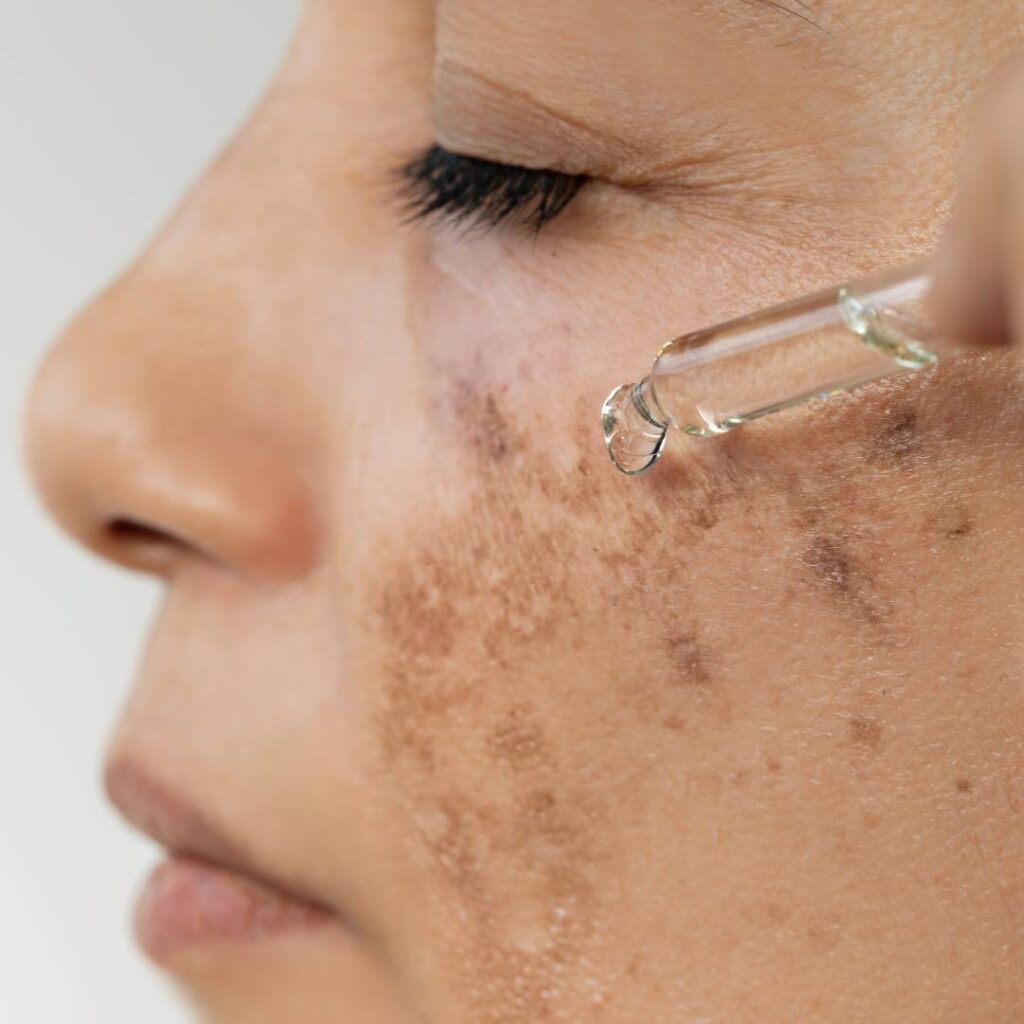
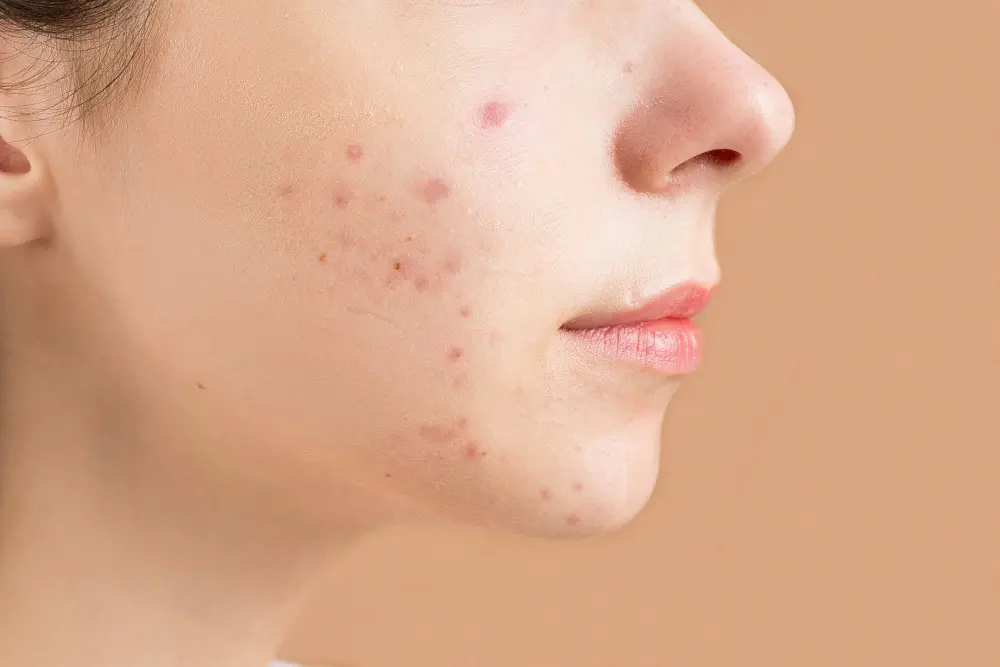
3. What Does PIH Look Like?
PIH is usually:
Flat (not raised)
Located exactly where the original bump/rash/injury was
Brown to dark brown most commonly
Sometimes gray or blue-gray (often indicates deeper pigment)
Tip: If a spot is raised, scaly, bleeding, changing rapidly, or not linked to a prior rash/blemish, it should be evaluated.
4. PIH vs Melasma
They can look similar, but they’re different:
PIH: follows inflammation (acne, eczema, bite) and matches the shape/location of the prior spot.
Melasma: tends to be symmetric patches on cheeks/forehead/upper lip and is strongly linked to sun + hormones.
Many people can have both.
5. How We Treat PIH
PIH treatment works best in layers: prevent new marks, fade existing marks, and protect the skin barrier.
5. a) Sun protection (foundation of PIH care)
Sun exposure can darken PIH and slow fading.
Daily broad-spectrum sunscreen
Hats / shade when outdoors
Consider protection from heat/visible light if you’re very pigment-prone
5. b) Treat the cause
If acne or eczema is still active, we focus on controlling it to prevent new marks.
5. c) Gentle brightening + skin barrier support
Common approaches include:
Prescription or medical-grade brighteners
Gentle retinoid routines (when appropriate)
Barrier repair moisturizers to reduce irritation
5. d) In-office options (selected patients)
When appropriate and safe for your skin type:
Chemical peels (carefully selected)
Other targeted procedures
Important: Over-treating or irritating the skin can worsen PIH—especially in pigment-prone skin—so we choose treatments carefully.
6. Pre-Op Instructions
(Not surgery—these are “before starting treatment or procedures” tips.)
Before your PIH visit
Bring a list (or photos) of current skincare products
Tell us if you have a history of dark marks after irritation or prior procedures
Avoid tanning/sunburn before your visit
If you’re treating acne: avoid picking/squeezing (a major PIH trigger)
If you’re scheduled for an in-office procedure (peel, etc.)
Avoid waxing/threading on the area beforehand (we’ll give timing)
Stop harsh exfoliants/strong acids/retinoids as directed
Let us know about:
Recent breakouts, eczema flares, or skin irritation
Pregnancy/breastfeeding (may change treatment options)
7. Post-Op Instructions
After starting topical treatment
Use products exactly as directed—more is not better
Expect gradual improvement over weeks to months
If you develop burning, significant redness, peeling, or worsening darkening, stop the product and contact the office
After an in-office treatment
Be strict with sun protection
Use gentle cleanser + bland moisturizer until healed
Avoid picking, scrubbing, or exfoliating until cleared
Call if you have increasing pain, swelling, blistering, pus, or fever
8. How Long Does PIH Take to Fade?
It depends on:
How deep the pigment is
Your skin tone and how reactive your pigment cells are
Ongoing sun exposure
Whether inflammation (acne/eczema) is still active
Some marks fade in weeks, others take months—and deeper gray/blue pigment can take longer.
Frequently Asked Questions
Is Post-Inflammatory Hyperpigmentation (PIH)a scar?
Usually no. PIH is a color change, not a texture change. True scars cause indentation or thickening.
Why do my acne marks last so long?
Inflammation stimulates pigment production. Picking, deeper acne, and sun exposure can make marks darker and longer-lasting.
Can PIH be prevented?
Often, yes. The best prevention is:
Treat acne/eczema early
Avoid picking/scratching
Daily sunscreen
Gentle skincare that protects the barrier
Should I use bleaching creams?
Some lightening ingredients can help, but “strong” or unregulated products can irritate skin and worsen PIH. It’s safest to use a dermatologist-guided plan.
Do chemical peels help PIH?
They can help in selected patients, but they must be chosen carefully—especially for pigment-prone skin—because irritation can trigger more PIH.
Why did my dark marks get darker after a product or treatment?
If the skin becomes irritated or inflamed, pigment can increase. This is why we focus on gentle, consistent treatment and barrier repair.
When should I be worried that it’s not PIH?
Schedule evaluation if a spot is:
Growing, bleeding, crusting, painful, or changing quickly
Not connected to a prior pimple/rash/injury
A new dark lesion that looks different from others
