 Non-Cancer Growths
Non-Cancer Growths
• Lipomas (Fatty Lumps)
What They Are and How We Treat Them
A lipoma is a common, non-cancerous (benign) lump made of fatty tissue that grows slowly under the skin. Lipomas are usually soft, movable, and painless. Many people choose to leave them alone—but removal is an option if a lipoma is bothersome, growing, or uncomfortable.
Good news: Most lipomas are harmless and can often be removed with a quick in-office procedure.
What Does a Lipoma Feel Like?
Lipomas often:
Feel soft or “doughy”
Move slightly when you press on them
Grow slowly over months or years
Are usually painless (but can cause discomfort if pressing on nerves or in a high-friction area)
Common locations: neck, shoulders, back, arms, thighs, and abdomen.
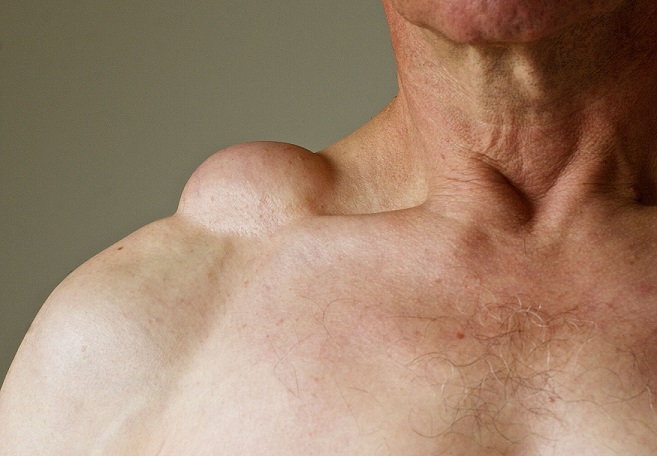
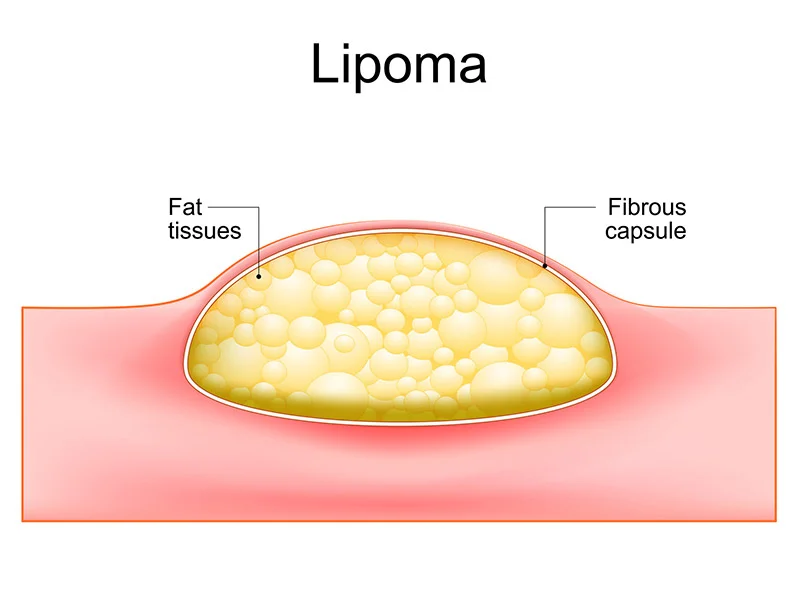
When Should You Get a Lump Checked?
Any new or changing lump should be evaluated—especially if it:
Is growing quickly
Is painful
Feels firm, fixed, or deeper in the tissue
Causes numbness/tingling
Appears with skin changes (redness, warmth, drainage)
Sometimes a lump that seems like a lipoma can be a cyst, enlarged lymph node, or another growth that needs a different approach.
How Lipomas Are Diagnosed
Diagnosis often starts with a simple office exam. If the lump has unusual features (deep, fast-growing, firm, painful), we may recommend:
Ultrasound (often the first imaging choice)
MRI (for deeper or more complex lumps)
Biopsy or removal if diagnosis is uncertain
Treatment Options
Watch and Monitor
If it’s small and not bothersome, monitoring is reasonable.
In-Office Removal (Excision)
The most common and definitive treatment is surgical excision:
Local numbing medicine (you’re awake)
A small incision
The lipoma is removed
Stitches may be placed
The tissue is often sent to pathology for confirmation
Most patients return to normal activities quickly with a few simple precautions.
Pre-Op Instructions (Before Lipoma Removal)
These are typical guidelines—your provider may adjust based on location and size.
1–2 weeks before (if applicable):
Tell us if you take blood thinners (warfarin, Eliquis, Xarelto, Plavix) or aspirin/NSAIDs.
Let us know about supplements that may increase bleeding (fish oil, vitamin E, ginkgo, garlic pills, turmeric).
Share any history of keloids, poor wound healing, or reactions to numbing medicine.
The day before / day of:
Shower and arrive with clean skin (no lotion on the area).
Wear loose, comfortable clothing that won’t rub the site.
Eat normally unless we give different instructions.
If the area is hairy, don’t shave the day of (it can irritate the skin). We’ll guide you if trimming is needed.
Plan ahead:
If your lipoma is large or in a spot that limits movement, consider arranging a ride and keeping your schedule light afterward.
Post-Op Instructions (After Lipoma Removal)
What to Expect
Mild soreness, tightness, or bruising for a few days
Small amount of spotting on the bandage the first day
A scar that fades gradually over months
Wound Care (Typical)
Keep the bandage on and the area dry for 24 hours (or as instructed).
After 24 hours, you may gently wash with soap and water. Pat dry.
Apply a thin layer of petroleum jelly (Vaseline/Aquaphor) unless told otherwise.
Replace with a clean bandage daily until healed.
Activity
Avoid heavy lifting, strenuous exercise, or stretching the area for 3–14 days, depending on location and size.
If the lipoma was on the back, shoulder, arm, or thigh, movement restrictions may be more important.
Pain Control
Most patients do well with acetaminophen (Tylenol).
Avoid aspirin/ibuprofen/naproxen for the first 24–48 hours unless your doctor says it’s okay, since these can increase bruising.
Call Us Right Away If You Notice:
Increasing redness, warmth, swelling, or worsening pain after day 2–3
Pus-like drainage or bad odor
Fever or chills
Bleeding that soaks through the dressing and doesn’t stop with firm pressure
The wound edges separate
Scar Care (After the Skin Has Sealed)
Once fully closed, consider:
Silicone gel or silicone sheets daily for 6–12 weeks
Daily sunscreen over the scar (SPF 30+) to reduce darkening
Schedule an Evaluation
If you have a new lump—or one that’s growing, painful, or changing—schedule an exam so we can confirm what it is and discuss your best options.
Frequently Asked Questions
Are lipomas dangerous?
Most lipomas are benign and not dangerous. We still recommend evaluation of any new or changing lump.
Can a lipoma turn into cancer?
A typical lipoma does not usually become cancer. Rarely, a different tumor type can mimic a lipoma—this is why we evaluate lumps that are growing quickly, painful, or firm.
Do lipomas go away on their own?
They usually do not disappear. Some stay the same size for years; others slowly enlarge.
Why remove a lipoma if it’s benign?
- Discomfort or pressure
- Rapid growth or uncertainty of diagnosis
- Cosmetic concerns
- Irritation from clothing or movement
Is lipoma removal painful?
The procedure is done with local anesthesia, so you should feel pressure but not sharp pain. Mild soreness afterward is common.
Will it leave a scar?
Yes—any incision can scar. We aim for the smallest practical incision and provide scar-care guidance to help it fade.
Can a lipoma come back after removal?
If removed completely, recurrence is uncommon, but it can happen—especially with larger or deeper lipomas.
Will you send it to the lab?
Often, yes. Many practices send removed tissue to pathology to confirm the diagnosis.
How long is recovery?
Many people return to normal routines within 1–2 days, but exercise or heavy lifting may be limited for several days to two weeks, depending on the site.
Is removal covered by insurance?
If removal is medically necessary (pain, growth, functional issues, or concern for diagnosis), it may be covered. Cosmetic removals may not be.

 Skin Cancer & Pre-Cancer Care
Skin Cancer & Pre-Cancer Care Medical Dermatology
Medical Dermatology Pigment & Lesion Disorders
Pigment & Lesion Disorders
 Cosmetic Dermatology
Cosmetic Dermatology